Research Article Open Access
Weight Loss Following Left Gastric Artery Embolization in a Human Population without Malignancy: A Retrospective Review
| Kevin Anton*, Tariq Rahman, Ashok B. Bhanushali, Luis L. Nadal, Gregory Pierce and Aalpen A. Patel | |
| Division of Vascular and Interventional Radiology, Department of Radiology, Geisinger Medical Center, Danville, USA | |
| Corresponding Author : | Kevin Anton Division of Vascular and Interventional Radiology Department of Radiology, Geisinger Medical Center Danville, PA 17822, USA Tel: 570-271-6203 Fax: 570-271-5976 E-mail: kfanton@geisinger.edu |
| Received November 22, 2015; Accepted November 30, 2015; Published December 03, 2015 | |
| Citation: Anton K, Rahman T , Bhanushali AB, Nadal LL, Pierce G, et al. (2015) Weight Loss Following Left Gastric Artery Embolization in a Human Population without Malignancy: A Retrospective Review. J Obes Weight Loss Ther 5:285. doi:10.4172/2165-7904.1000285 |
|
| Copyright:© 2015 Anton K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
| Related article at Pubmed, Scholar Google | |
Visit for more related articles at Journal of Obesity & Weight Loss Therapy
Abstract
Objective: Recent evidence suggests embolization of the left gastric artery, which provides the predominant arterial supply to the gastric fundus, may affect energy homeostasis through alterations in ghrelin production. The purpose of this study is to evaluate post-procedural weight loss following left gastric artery embolization (performed for reasons other than for weight loss) in patients without malignancy. Materials and Methods: A retrospective review of patients who underwent arterial embolization for acute upper gastrointestinal hemorrhage between January 2002 and January 2014 was conducted. A study group of 10 patients who underwent left gastric artery embolization and control group of 22 patients who underwent embolization of a different mesenteric or visceral arterial branch for non-tumoral acute gastrointestinal bleeding were collected. Their electronic medical records were reviewed and data points for height, weight, and body mass index were collected at 1-, 4-, 8-, and 12-month post-procedural time points. Exclusion criteria included age less than 18 years and documented history of malignancy. Results: The left gastric artery embolization group had a significantly greater reduction in body mass index compared with the control group at 1 month (-9.8% vs. -4.0%, p=0.042) and 4 months (-11.7% vs. +0.1%, p=0.033). No significant change was demonstrated at 8 months (-8.6% vs. -1.7%, p=0.32) and 1 year (-5% vs. +2.6%, p=0.42) compared with controls. Conclusion: Left gastric artery embolization provides early post-procedural weight loss that may persist for at least 1 year. Further studies will better elucidate the role of gastric artery embolization in the management of bariatric patients.
| Keywords |
| Gastric artery; Malignancy; Embolization |
| Introduction |
| Morbidity and mortality associated with obesity has become a health care epidemic as average body mass index (BMI) continues to trend higher globally [1]. |
| Lifestyle changes including diet and exercise can be beneficial for some; however maintenance of weight loss proves difficult as many people regain most, if not all, of their lost weight. Invasive procedures, such as Roux-en-y gastric bypass, sleeve gastrectomy, and gastric lap banding all provide significant weight loss in those who also make lifestyle changes [2-4]. Post-procedural complications have decreased with laparoscopic techniques but when they occur, still can be debilitating, leading to significant increases in hospital stays and health care costs [5]. Medical management has yet to offer a substantial drug candidate although numerous candidates are in the pipeline [6]. |
| As the age of invasive surgery transitions to minimally-invasive approaches, there is an opportunity for bariatric embolization to become incorporated into the treatment algorithm for weight loss. Through alterations in gut hormone production and secretion, left gastric artery embolization has been shown, in animal models, to influence energy homeostasis towards a state of reduced appetite and weight loss [7,8]. Retrospective human evidence in patients undergoing left gastric artery embolization (LGAE) for acute upper gastrointestinal (GI) hemorrhage and ongoing prospective studies further evaluating the technique for weight loss will continue to define its feasibility. |
| Materials and Methods |
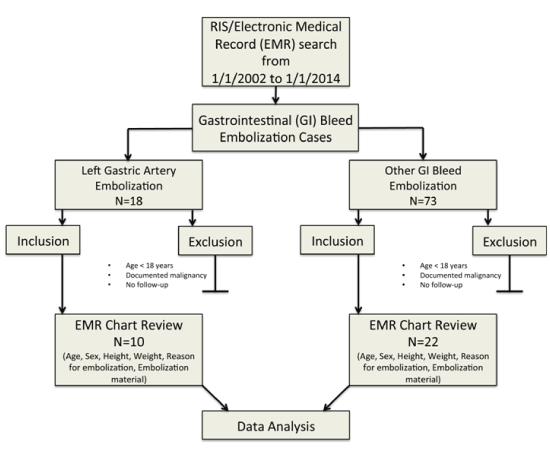
| Following IRB approval, a retrospective review of patients who underwent arterial embolization for acute gastrointestinal hemorrhage between January 2002 and January 2014 was conducted. An initial search for patients over 18 years of age with prior embolization for gastrointestinal bleeding was conducted through RIS (Radiology Information System) and the electronic health records system using keywords in medical records and radiology reports. In addition, current procedural terminology (CPT) codes were used to search for patients with GI bleed within the approved timeframe. A total of 91 patients were identified (Figure 1). |
| The electronic medical records of this patient population were reviewed and subdivided into patients who underwent left gastric artery embolization (n=18) or embolization of a different visceral or mesenteric vessel (n=73). Additional medical chart analysis excluded patients with a documented history of malignancy or lack of postprocedural follow-up. A final study group of 10 patients who underwent LGAE and control group of 22 patients who underwent embolization of a different visceral or mesenteric artery branch for non-tumoral acute gastrointestinal bleeding were identified. Height and weight values for each patient were collected at pre-procedural and 1 month, 4 month, 8 month, and 12 month post-procedural time points. BMI was calculated using the National Institutes of Health (NIH) BMI calculator. |
| Additional collected data points included indication for the procedure and embolization material. Statistical analysis was conducted using student’s t-test with a p-value <0.05 considered to be significant. |
| Results |
| Patient population |
| The LGAE group (N=10) was comprised of 7 males and 3 females with an average age of 55.8 years (36 to 79 years) and average BMI of 31 (22 to 45) (Table 1). The control group (N=22) was comprised of 12 males and 10 females with an average age of 70.7 years (23 to 92 years) and average BMI of 28.4 (20.8 to 45.6). |
| Embolization characteristics |
| The LGAE group was composed of patients who underwent LGAE for non-malignancy related acute upper gastrointestinal bleeding. Embolization material included coils (N=5), gelatin sponge pledget suspension/slurry (N=3), or a combination of coils and gelatin sponge pledget suspension/slurry (N=2) (Table 2). Control group patients underwent embolization of any visceral or mesenteric artery branch, except the left gastric artery, for acute gastrointestinal bleeding. Arterial branches embolized in the control group included the gastroduodenal artery (N=9), right hepatic artery (N=1), pancreaticoduodenal artery (N=2), right gastroepiploic artery (N=1), branches of the cecal artery (N=1), inferior pancreaticoduodenal artery (N=1), inferior mesenteric artery (N=3), right colic artery (N=3), and middle colic artery (N=1). Embolization material in the control group included coils (N=17), gelatin sponge pledget suspension/slurry (N=3), a combination of coils and gelatin sponge pledget suspension/slurry (N=1), and embospheres (N=1) (Table 3). Embolization material was selected based on operator preference and individual case characteristics. |
| Body mass index measurements |
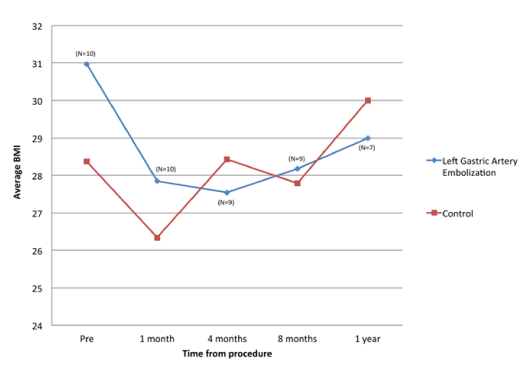
| Pre-procedural body mass index (BMI) values were not significantly different between the LGAE (BMI 31 ± 6.8) and control groups (BMI 28.4 ± 6.4) (p=0.32). BMI in both the LGAE (N=10) and control groups decreased at 1-month post-embolization (27.9 ± 6 and 26.3 ± 6.6, respectively). At later time points (4-, 8-, and 12-months post-embolization), BMI returned to pre-embolization levels in the control group (28.4 ± 6.4 at 4 months, 27.8 ± 6.7 at 8 months, and 30.0 ± 7.3 at 12 months). In the LGAE group, BMI remained below preembolization levels at 4-months (27.5 ± 6.7, N=9), 8-months (28.2 ± 6.5, N=9), and 12-months (29 ± 7.1, N=7) (Figure 2). |
| The LGAE group demonstrated a greater reduction in BMI compared with the control group at 1 month (-9.8% vs. -4.0%, p=0.042) and 4 months (-11.7% vs. +0.1%, p=0.033) post embolization (Figure 3). No statistically significant reduction at 8 months (-8.6% vs. -1.7%, p=0.32) or 1 year (-5% vs. +2.6%, p=0.42) was demonstrated. No data was available for 3 of 10 study patients at 1-year post procedure. Sample size was too small to evaluate for significant differences in weight loss with respect to embolization material including coils, gelatin sponge, or a combination of coils and gelatin sponge. |
| In the post-procedural follow-up period none of the study patients enrolled in a dedicated weight loss program or significantly altered their diet or exercise routine as could be evaluated through the electronic medical record. No patient experienced a repeat episode of upper GI bleeding. One patient experienced two episodes of lower GI bleeding, documented by colonoscopy. Multiple patients were hospitalized for various non-GI bleeding related illnesses in the year following their LGAE (Table 4). |
| Discussion |
| The rationale for transarterial left gastric artery embolization as a specific means for weight loss stems from the role gut hormones, such as ghrelin, play in appetite and energy homeostasis [9]. Recent data evaluating gut hormones following bariatric surgery suggest that these alterations in humoral signaling may be partially responsible for post procedural weight loss [10-12]. Initial animal studies demonstrated early reduction in circulating ghrelin levels and decreased weight gain in developing swine [7,8,13,14]. |
| A retrospective review of 19 patients who underwent left gastric artery embolization for gastrointestinal bleeding found on average, a 7.3% reduction in body weight after 3 months compared with a 2% decrease in the control group [15]. The study included patients with malignancy with a known predisposition to rapid changes in weight. If more patients in the LGAE group had active or more aggressive malignancy during the study period, their changes in weight may not be directly related to the embolization. In our study, patients with a documented history of malignancy prior to embolization or during the follow up period were excluded to remove the potential weight loss bias of active malignancy. |
| Kipshidze, et al. presented the first human data evaluating 5 patients treated with LGAE at the American College of Cardiology meeting in 2013[16]. They demonstrated an average weight loss of 45 pounds at 6-months post-procedure. Additional larger phase 1 followed by phase 2/3 trials with long-term follow up will be necessary to better elucidate the role of gastric artery embolization in the management of bariatric patients. Some of the early ongoing trials include the Gastric Artery Embolization Trial for Lessening Appetite Nonsurgically (GETLEAN) and the Bariatric Embolization of Arteries for the Treatment of Obesity (BEAT Obesity). As the bariatric embolization technique evolves, additional studies evaluating embolization material, degree of embolization, and follow up of long-term occlusion (recanalization and/or collateral vascularization) will become important. |
| There were multiple limiting factors affecting the results of this study. This was a single-institution analysis of left gastric artery embolization for acute upper gastrointestinal bleeding in a population without documented history of malignancy. Following exclusion of patients not meeting the inclusion criteria, our sample size was small which limited study power and statistical significance, particularly at later time points. Due to low sample size and non-standardized follow-up, only 7 of the initial 10 LGAE patients had data points available at the 12-month time point. The retrospective nature of the study inherently provides less robust data when compared with a standardized, prospective, randomized control trial. We were therefore unable to match all potentially confounding factors between the study and control groups. In addition, evaluation of the serum ghrelin level, as was conducted in prior animal studies, was not feasible. |
| The durability of left gastric artery embolization should be a topic of significant interest. In both our study and the prior studies evaluating LGAE, weight changes were trending back towards baseline between 6 and 12 months. Also, in the prior studies evaluating LGAE where ghrelin levels were obtained, ghrelin levels were trending back towards baseline between 6 and 12 months. This may be partially due to the use of gelatin sponge and its temporary occlusive effect, allowing for recanalization within weeks to months [17]. Embolization particle size and the degree of embolization (stasis, near stasis, etc.) will likely affect both early weight loss and longer term durability. Future studies should evaluate multiple particle sizes and varying degrees of embolization to refine the procedural techniques, promoting optimal outcomes. |
| Despite the described limitations, the data suggest that embolization of the left gastric artery leads to early weight loss and prolonged time below baseline weight. |
| Conclusion |
| Left gastric artery embolization provides early post-procedural weight loss that may persist for at least 1 year. However, further studies will better elucidate the role of gastric artery embolization in the management of bariatric patients. |
References
- Finucane MM, Stevens GA, Cowan MJ, Danaei G, Lin JK, et al. (2011)National, regional, and global trends in body-mass index since 1980: systematic analysis of health examination surveys and epidemiological studies with 960 country-years and 9.1 million participants. Lancet37: 557-67.
- Dixon JB, Straznicky NE, Lambert EA, Schlaich MP, Lambert GW (2012) Laparoscopic adjustable gastric banding and other devices for the management of obesity. Circulation 126: 774-85.
- Vest AR, Heneghan HM, Schauer PR, Young JB (2013) Surgical management of obesity and the relationship to cardiovascular disease. Circulation 127: 945-959
- Kushner RF(2014)Weight loss strategies for treatment of obesity. Progress in cardiovascular diseases 56: 465-72.
- Reoch J,Mottillo S, Shimony A, Filion KB, Christou NV,et al. ( 2011) Safety of laparoscopic vs open bariatric surgery: a systematic review and meta-analysis. Arch Surg 146: 1314-22.
- Kakkar AK, Dahiya N (2015) Drug treatment of obesity: current status and future prospects. Eur J Intern Med 26: 89-94.
- Arepally A,Barnett BP, Patel TH, Howland V, Boston RC,et al. (2008) Catheter-directed gastric artery chemical embolization suppresses systemic ghrelin levels in porcine model. Radiology 249: 127-33
- Paxton BE, Kim CY, Alley CL, Crow JH, Balmadrid B, et al. (2013) Bariatric embolization for suppression of the hunger hormone ghrelin in a porcine model. Radiology 266: 471-9.
- Kaiyala KJ, Woods SC, Schwartz MW (1995) New model for the regulation of energy balance and adiposity by the central nervous system. Am J Clin Nutr 62: 1123S-1134S.
- Perry B, Wang Y(2012) Appetite regulation and weight control: the role of gut hormones. Nutr Diabetes 2: e26
- Murphy KG, Bloom SR (2004) Gut hormones in the control of appetite. Exp Physiol 89: 507-516
- Cummings DE, Overduin J(2007) Gastrointestinal regulation of food intake. J Clin Invest 117: 13-23
- Arepally A, Barnett BP, Montgomery E, Patel TH (2007) Catheter-directed gastric artery chemical embolization for modulation of systemic ghrelin levels in a porcine model: initial experience. Radiology 244: 138-143
- Paxton BE, Alley CL, Crow JH, Burchette J, Weiss CR,et al. (2014) Histopathologic and immunohistochemical sequelae of bariatric embolization in a porcine model. Journal of vascular and interventional radiology 25: 455-461
- Gunn AJ, Oklu R (2014)A preliminary observation of weight loss following left gastric artery embolization in humans. J Obes 2014: 185349.
- Kipshidze N,Archvadze A, Kantaria M(2013) First–In–Man study of left gastric artery embolization for weight loss. Journal of the American College of Cardiology
- Vaidya S,Tozer KR,Chen J(2008) An overview of embolic agents. Semin Intervent Radiol 25: 204-215.
Tables and Figures at a glance
| Table 1 | Table 2 | Table 3 | Table 4 |
Figures at a glance
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 |
Relevant Topics
- Android Obesity
- Anti Obesity Medication
- Bariatric Surgery
- Best Ways to Lose Weight
- Body Mass Index (BMI)
- Child Obesity Statistics
- Comorbidities of Obesity
- Diabetes and Obesity
- Diabetic Diet
- Diet
- Etiology of Obesity
- Exogenous Obesity
- Fat Burning Foods
- Gastric By-pass Surgery
- Genetics of Obesity
- Global Obesity Statistics
- Gynoid Obesity
- Junk Food and Childhood Obesity
- Obesity
- Obesity and Cancer
- Obesity and Nutrition
- Obesity and Sleep Apnea
- Obesity Complications
- Obesity in Pregnancy
- Obesity in United States
- Visceral Obesity
- Weight Loss
- Weight Loss Clinics
- Weight Loss Supplements
- Weight Management Programs
Recommended Journals
Article Tools
Article Usage
- Total views: 10696
- [From(publication date):
December-2015 - Apr 03, 2025] - Breakdown by view type
- HTML page views : 9837
- PDF downloads : 859
