Case Report Open Access
Subdural Hematoma Infected with Escherichia coli in a 5-Month-Old Male Infant: Case Report
| Yu-Lung Hsu1, Hsiao-Chuan Lin1, Yu-Tzu Chang2, Hsiang-Ming Huang3, Tsung-Hsueh Hsieh1, Ting-Yu Yen1, Hsiu-Mei Wei1 and Kao-Pin Hwang1* | ||
| 1Department of Pediatric Infectious Diseases, Children’s Hospital, China Medical University Hospital, China Medical University School of Medicine, Taichung, 40402, Taiwan | ||
| 2Department of Pediatric Neurology, Children’s Hospital, China Medical University Hospital, China Medical University School of Medicine, Taichung, 40402, Taiwan | ||
| 3Department of Neurosurgery, China Medical University Hospital, China Medical University School of Medicine, Taichung, 40402, Taiwan | ||
| Corresponding Author : | Kao-Pin Hwang Department of Pediatric infectious disease Children’s Hospital, China Medical University Hospital China Medical Universityn School of Medicine, #2 Yuh-Der Road, Taichung 40447, Taiwan Tel: +886-4-2205-2121(1930) E-mail: kapihw@mail.cmuh.org.tw |
|
| Received February 25, 2015, Accepted March 27, 2015, Published April 03, 2015 | ||
| Citation: Hsu YL, Lin HC, Chang YT, Huang HM, Hsieh TH, et al. (2015) Subdural Hematoma Infected with Escherichia coli in a 5-Month-Old Male Infant: Case Report. J Infect Dis Ther 3:209. doi: 10.4172/2332-0877.1000209 | ||
| Copyright: © 2015 Hsu YL, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | ||
Related article at Pubmed Pubmed  Scholar Google Scholar Google |
||
Visit for more related articles at Journal of Infectious Diseases & Therapy
Abstract
Hematogenous dissemination from a localized infection to a previous existing subdural hematoma is an extremely rare cause of subdural empyema which is termed infected subdural hematoma. We reported a 5-month-old male infant suffered from infected subdural hematoma by Escherichia coli (E. coli). In this patient, urinary tract infection was the most favorable origin from which seed the organism to subdural space hematogenously with evidence of pyuria and pyelonephritis. Subdural empyema was well treated after burr hole drainage with adequate antibiotic use. This infant is now doing well based on findings from regular outpatient followed-up without recurrence of infection and sequela. In conclusion, the applicable treatment strategy for infected subdural hematoma has not been determined due to its rarity. However, adequate drainage and duration of antibiotic use will be related to achieving a more satisfactory outcome when compared with subdural empyema associated with meningitis.
| Keywords | |
| Escherichia coli ; Infant; Infected subdural hematoma; Subdural empyema | |
| Introduction | |
| Subdural empyema (SDE) means that the infection occurred in the space between the dura and arachnoid. It is a serious central nervous system infection related to further neurological sequelae and in some cases even death [1]. Infections from the otorhinolaryngeal region, including paranasal sinus, inner ear and mastoid, are the most common origins to cause subdural empyema [2]. Hematogenous dissemination from a localized infection to a previous existing subdural hematoma is an extremely rare cause of subdural empyema which is termed infected subdural hematoma [3]. | |
| We report a 5-month-old male infant with subdural hematoma containing purulent material associated with Escherichia coli infection which may translocate from a urinary tract infection. | |
| Case Report | |
| A 5-month-old previous healthy male infant was admitted to our hospital with the chief complaint of high fever for 2 days. The patient was born at 37 weeks of gestational age and the delivery was smooth and normal. He reached the appreciated developmental milestones and did well with good overall activity and feeding. Upon physical examination, no specific abnormality was found except for fever. Laboratory examination disclosed peripheral white blood cell count 18,020/μL (normal range: 6,000-14,000/μL), red blood cell count 408 × 104/μL (normal range: 310 × 104-450 × 104/μL), hemoglobin concentration 11.1 gm/dl (normal range: 10.5-14.0 gm/dl), hematocrit 31.9% (normal range: 32-42%), platelet count 36.6 x 104/μL (normal range: 15.0 × 104-40.0 × 104/μL), C-reactive protein (CRP) concentration 32.0 mg/dl (normal range: 0.08-1.12 mg/dl). Urinary analysis revealed white blood cell count 54/μL (normal range: <28/μL), red blood cell count 326/μL (normal range: <17/μL) and protein 30 mg/dL (normal range: negative). Renal echogram showed positive findings of cystitis and left pelviectasis which was proven to be diagnosed as acute pyelonephritis. Therefore, cefazolin (100 mg/kg/day Q8H) and gentamicin (2.5 mg/kg/dose Q8H) were prescribed. | |
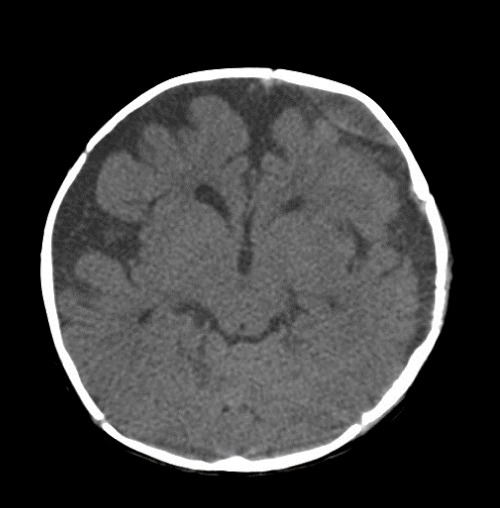
| On the second day of admission, irritable crying and focal seizure localized on the infant’s right side extremities were noted. Emergent cranial computed tomography (CT) demonstrated biconvex-shaped fluid collection beneath the left frontal bone, increased enhancement and mild thickening on the dura of left hemisphere without of the midline shift (Figure 1). The preoperative diagnoses were chronic subdural hematoma and subdural empyema of left frontal, parietal and temporal regions. Burr-hole surgery revealed a hematoma with thick and pinkish-red outer membrane. Aspiration was performed and the fluid was purulent, yellowish-white color that was foul-smelling. The subdural space was irrigated with a sterile saline solution and a drain was set. E. coli was isolated from the purulent fluid by bacterial culture. After operation, this infant was treated with third-generation cephalosporin (cefotaxime 200 mg/kg/day Q6H) intravenously. | |
| There were no bacteria isolated in the urine and blood soon after admission. Because of the findings of pyuria and acute pyelonephritis, urinary tract infection was considered to be the most likely origin of seeding hematogeously to the subdural space. | |
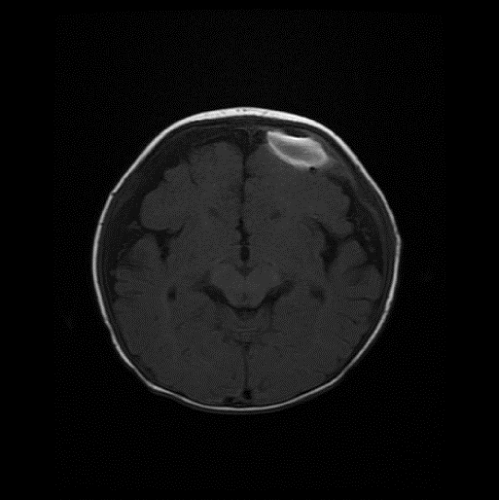
| The patient became afebrile on the second day after operation. Magnetic resonance image performed 11 days after the first operation demonstrated a loculated biconvex fluid collection beneath the left frontal bone and crescent-shaped hypointense fluid accumulated in the bilateral subdural space on T1-weighted image (Figure 2). A second operation was performed 12 days after the first operation to drain the residual purulent fluid. The subdural space was irrigated again with sterile saline solution and a drain was set again. Aspiration fluid was sent for bacterial culture with negative findings. Subdural drain was removed 10 days after operation. | |
| The total duration of antibiotic use was 4 weeks. The patient discharged without neurologic deficits. Oral third generation cephalosporin (ceftibuten 9 mg/kg/day BID) was given for an additional 3 weeks. To date the patient is doing based on regular outpatient followed-up for 6 months without recurrence of infection and sequela. | |
| Discussion | |
| Subdural hematoma (SDH) represents bleeding into the spaces between dura and arachnoid space. According to the time from onset, SDH can be categorized into acute, subacute and chronic, which presented one to two days, 3 to 14 days, and 15 or more days after onset respectively. Acute SDH is characterized by fresh blood clot and is mostly fluid. Subacute SDH is typified by encapsulation of the blood clot with a thick outer membrane and a thinner inner membrane due to dural collagen synthesis. Chronic SDH is yellowish-brown color because there is often small central unresorbed blood [4]. | |
| The incidence of subdural hematoma is 24 per 100,000 infants under one year of age. Most SDH is disclosed below 4 months of age. Birth trauma is an important cause of SDH. The location of birth related SDH commonly occurs in the posterior fossa or over the posterior part of the brain, rarely on the isolated supratentorial area [5]. A study of the natural history of neonatal SDH by magnetic resonance imaging (MRI) revealed that haematomas are generally completely resolved 4 weeks after birth [6]. Head injury is still the most common cause of SDH. However, tracing back the history of our patient, his families denied any traumatic episodes. The cause of chronic SDH of this infant remains unclear. | |
| Subdural empyema is estimated to account for 15-25% of childhood localized intracranial bacterial infections [7]. The most common condition predisposing to cranial subdural empyema is otorhinologic infections, especially paranasal sinusitis [8] and/or bacterial meningitis [9]. However, in the present case, these predisposing factors cannot be identified. | |
| Hematogenous seeding from a distant infection to the subdural space is quite unusual. Thus, we consider this subdural empyema was hematogenously infected to the previous hematoma based on the following two findings. First, there were no predisposing factors for subdural empyema such as otorhinolaryngeal infections, meningitis, head trauma, or suffering from previous neurosurgical procedure. Second, the subdural space is clear; therefore, pus could be extended widely to the surface of the brain. However, during operation, inner and outer membranes of the empyema were encapsulated and limited the spread of pus. Yellowish-brown color within thickened outer membrane also supported the presence of chronic SDH [3]. | |
| In this case, Escherichia coli were identified as the causative organism of subdural empyema. Besides, there were no other sources of infection that could be traced. In view of the pyuria and the findings of the renal echogram on admission, the origin of hematogenous seeding to cause the subdural empyema was postulated to be the urinary tract infection. A report collected 14 cases of infected subdural hematomas, and none of them were noted as having postoperative complications. In twelve of the 14 cases, the possibility of secondary hematogenous seeding of a previous existing subdural hematoma was suggested. The most common contributing pathogen was E. coli (5/14, 35.7%). The original infection sources included the urinary tract infection (n=3), gastrointestinal disease (n=3), meningitis (n=1), ethmoiditis (n=1), and unknown (n=6). In two of five E. coli infection cases, their pathogen originated from the urinary tract [10]. | |
| Even with improvements in diagnostic techniques and therapeutic management, reported mortality rates of SDE range from 0 to 12%. In Taiwan, a study revealed the mortality rate was 9.7%. All of the cases in which patients expired suffered from pneumococcal meningitis complicated with related SDE [2]. The treatment purpose of SDE is to drain the pus and eradicate the source of infection. Drainage by the burr-hole method or craniotomy has been used. A study concluded that drainage with burr-hole should be considered as an effective and safe method for post-meningitis SDE in infants when detected early [11]. However, the number of cases of infected subdural hematoma remains rare, and as a result the applicable treatment strategy has not been firmly established to date. Of the previously reported cases which included both children and adults, nine of them received burr-hole drainage; four by craniotomy. Only one adult case received a craniotomy after burr-hole method. Ten of the 14 cases recovered without neurologic deficits [10]. Another report of infant patients highlighted that they were also successfully treated by empiric antibiotics and burr-hole drainage [12]. In this case, we also selected burr-hole drainage due to its less invasive nature. According to a study with 20-years of experience in a medical center, the mean duration of antibiotic therapy for SDE was 36.8 ± 14.2 days (range, 9 to 56 days) [2]. Our case received antibiotics for 7 weeks. Burr-hole drainage and adequate subdural irrigation followed by antibiotic therapy made the patient free of infection successfully. | |
| In conclusion, hematogenous disseminatation from a distant infection to a pre-existing subdural hematoma is an extremely rare cause of subdural empyema. It can be successfully treated by burr-hole drainage and a sufficient duration of antibiotic use. | |
References
- Dill SR, Cobbs CG, McDonald CK (1995) Subdural empyema: analysis of 32 cases and review. Clin Infect Dis 20: 372-386.
- Wu TJ, Chiu NC, Huang FY (2008) Subdural empyema in children--20-year experience in a medical center. J Microbiol Immunol Infect 41: 62-67.
- Kawamoto S, Nagata K, Mochizuki Y, Hara T, Abe T, et al. (1998) Subdural empyema caused by hematogenous dissemination from an abscess in thigh to a preexisting chronic subdural hematoma--case report. Neurol Med Chir (Tokyo) 38: 743-745.
- Smith C (2006) Intracranial haemorrhage in infants. Current Diagnostic Pathology 12: 184-190.
- Squier W, Mack J (2009) The neuropathology of infant subdural haemorrhage. Forensic Sci Int 187: 6-13.
- Whitby EH, Griffiths PD, Rutter S, Smith MF, Sprigg A, et al. (2004) Frequency and natural history of subdural haemorrhages in babies and relation to obstetric factors. Lancet 363: 846-851.
- Bockova J, Rigamonti D (2000) Intracranial empyema. Pediatr Infect Dis J 19: 735-737.
- Adame N, Hedlund G, Byington CL (2005) Sinogenic intracranial empyema in children. Pediatrics 116: e461-467.
- Chang YC, Huang CC, Wang ST, Chio CC (1997) Risk factor of complications requiring neurosurgical intervention in infants with bacterial meningitis. Pediatr Neurol 17: 144-149.
- Sawauchi S, Saguchi T, Miyazaki Y, Ikeuchi S, Ogawa T, et al. (1998) Infected subdural hematoma. J Clin Neurosci 5: 233-237.
- Liu ZH, Chen NY, Tu PH, Lee ST, Wu CT (2010) The treatment and outcome of postmeningitic subdural empyema in infants. J Neurosurg Pediatr 6: 38-42.
- Iimura Y, Tsutsumi S, Mitome Y, Nonaka Y, Abe Y, et al. (2010) Infantile chronic subdural hematoma infected by Escherichia coli--case report. Neurol Med Chir (Tokyo) 50: 482-484.
Figures at a glance
 |
 |
|
| Figure 1 | Figure 2 |
Relevant Topics
- Advanced Therapies
- Chicken Pox
- Ciprofloxacin
- Colon Infection
- Conjunctivitis
- Herpes Virus
- HIV and AIDS Research
- Human Papilloma Virus
- Infection
- Infection in Blood
- Infections Prevention
- Infectious Diseases in Children
- Influenza
- Liver Diseases
- Respiratory Tract Infections
- T Cell Lymphomatic Virus
- Treatment for Infectious Diseases
- Viral Encephalitis
- Yeast Infection
Recommended Journals
Article Tools
Article Usage
- Total views: 14740
- [From(publication date):
April-2015 - Nov 21, 2024] - Breakdown by view type
- HTML page views : 10293
- PDF downloads : 4447
