Research Article Open Access
Skin Problems in the Lower Legs of Morbidly Obese Patients and the Possible Role of Bariatric Surgery
| William R Parkyn, Cheng Yee Chan and Andre M Van Rij* | |
| Department of Surgical Sciences, Dunedin School of Medicine, University of Otago, Dunedin, New Zealand | |
| Corresponding Author : | Andre M. Van Rij Department of Surgical Sciences Dunedin School of Medicine, University of Otago PO Box 56, Dunedin 9054, New Zealand Tel: +64 3 474 0999; Ext: 8834 Fax: +64 3 474 7622 E-mail: andre.vanrij@otago.ac.nz |
| Received August 21, 2014; Accepted September 25, 2014; Published September 30, 2014 | |
| Citation: Parkyn WR, Chan CY, Van Rij AM (2014) Skin Problems in the Lower Legs of Morbidly Obese Patients and the Possible Role of Bariatric Surgery. J Obes Weight Loss Ther 4:230. doi:10.4172/2165-7904.1000230 | |
| Copyright: © 2014 Parkyn WR, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Obesity & Weight Loss Therapy
Abstract
Objective: Anecdotally, lower leg skin changes in morbidly obese people appear much improved with weight loss following bariatric surgery. The objective of this study was to compare prevalence of lower leg symptoms in obese patients awaiting, and those who have had, bariatric surgery. Methods: An audit was undertaken, utilising questionnaires, to identify obesity-associated lower leg symptoms: swelling, itchiness, colour changes, hot/burning feeling, eczema and ulcers. There were three groups: those awaiting surgery (‘Obesity Clinic’), those who had surgery (‘Post-Surgery’), and those in ‘Post-Surgery’ recalling pre-operative symptoms (‘Pre-Surgery Recall’). Results: Participants totalled 117; 62 in ‘Obesity Clinic’ and 55 in ‘Post-Surgery’ (81.8% response rate). Overall prevalence of symptoms was significantly lower in ‘Post-Surgery’ (36.4%) compared to ‘Obesity Clinic’ (80.6%) and ‘Pre-Surgery Recall’ (74.5%) (p<0.0001). Individual symptoms were also similarly less prevalent. Conclusion: These results establish the high prevalence of lower leg skin changes in morbidly obese patients, which is significantly lower in those who have undergone bariatric surgery, possibly due to improved underlying venous stasis from decreased intra-abdominal pressure and weight. Decreased popliteal vein compression from weight loss, and weight reduction itself may also be contributing factors. This suggests a role for bariatric surgery in the potentially cost-effective treatment of lower leg symptoms in the morbidly obese.
Methods: An audit was undertaken, utilising questionnaires, to identify obesity-associated lower leg symptoms: swelling, itchiness, colour changes, hot/burning feeling, eczema and ulcers. There were three groups: those awaiting surgery (‘Obesity Clinic’), those who had surgery (‘Post-Surgery’), and those in ‘Post-Surgery’ recalling pre-operative symptoms (‘Pre-Surgery Recall’).
Results: Participants totalled 117; 62 in ‘Obesity Clinic’ and 55 in ‘Post-Surgery’ (81.8% response rate). Overall prevalence of symptoms was significantly lower in ‘Post-Surgery’ (36.4%) compared to ‘Obesity Clinic’ (80.6%) and ‘Pre-Surgery Recall’ (74.5%) (p<0.0001). Individual symptoms were also similarly less prevalent.
Conclusion: These results establish the high prevalence of lower leg skin changes in morbidly obese patients, which is significantly lower in those who have undergone bariatric surgery, possibly due to improved underlying venous stasis from decreased intra-abdominal pressure and weight. Decreased popliteal vein compression from weight loss, and weight reduction itself may also be contributing factors. This suggests a role for bariatric surgery in the potentially cost-effective treatment of lower leg symptoms in the morbidly obese.
There are over 500 million people with obesity worldwide [6]. Lower leg skin problems and ulceration appear to be a common, under-recognised co-morbidity of obesity, thus representing a large burden on the health system. They are very difficult to manage in terms of treatment, as the skin changes and ulcers tend to recur, probably due to the persistence of the underlying pathology, resulting in long periods of treatment by various modalities including dressings and topical and oral medications, and ongoing involvement with nursing and medical practitioners. The cost of treating obesity-related skin problems is likely to be similar to that of venous ulcers in the community.
Interestingly, obesity-related lower leg skin problems have been said to disappear following bariatric surgery, although this has also not been previously documented in the literature. Bariatric surgery, surgery carried out for the primary purpose of weight loss, is now increasingly recognised to procure many health benefits, some of which are independent of weight loss following surgery. There is evidence that bariatric surgery improves type II diabetes mellitus, hypercholesterolaemia, and hypertension, amongst other obesity-related conditions [7]. With regard to weight loss and diabetes in the context of obesity, bariatric surgery has been shown to be more effective than conventional treatments, and more cost-effective as well in the long term [8,9].
It may be that bariatric surgery also affects a cure on obesity-related skin problems in a clinically- and cost-effective manner. However, because there is currently nothing in the published literature documenting (1) the prevalence of skin changes in the lower legs of obese individuals, and (2) the effect of bariatric surgery on these skin changes, this study first aimed to establish if there is indeed any difference in the prevalence of skin changes in the lower legs of obese individuals before and after bariatric surgery.
Potential participants were posted a questionnaire, which included questions on current weight, and any problems they were currently experiencing in their legs, such as swelling, itchiness, colour changes, hot or burning feelings, eczema, ulcers or any other symptoms. A freepost envelope was included to facilitate their reply. Participants who had not responded after a month were sent a reminder. If they had not replied within a week of the reminder, they were telephoned, and the questionnaire was completed over the phone.
Two groups of patients were approached. The first group, the ‘Obesity Clinic’ group, included those awaiting bariatric surgery. The second group, termed the ‘Post-Surgery’ group, included those patients who had had a bariatric procedure in the three years prior to this study. In addition to filling out the questionnaire to determine current symptoms, patients in the second group were also requested to fill out a second questionnaire recalling the symptoms in their legs prior to surgery. Presence of varicose veins was established clinically from the clinical record in both groups. The recollection of symptoms prior to bariatric surgery was termed the ‘Pre-Surgery Recall’ group.
Height, pre-operative weight and other demographic information were obtained from clinical records. Body Mass Index (BMI) was calculated. Statistical analysis was performed using Chi-squared test for categorical data and t-test for continuous variables. This was done using StatView (version 5.0.1, SAS Institute Inc. 92-98). Significance was set at p<0.05.
In the Post-Surgery group, all patients had an open Roux-en-Y gastric bypass procedure. The average pre-operative weight was 153.5 ± 29.7 kg, and the average weight loss following surgery was 54.8 ± 20.9 kg, representing a BMI decrease of 19.6 ± 7.1 kg/m2. The median time from surgery was 18 (10-36) months (Table 1).
A major finding in this study is the observation that the prevalence of obesity-related skin problems was markedly lower in the Post-Surgery group, in comparison to the Obesity Clinic and Pre-Surgery Recall group. It may be inferred that bariatric surgery appears to be a factor in resolving skin changes that are often seen in the morbidly obese. Whether this is an effect that can be attributed to significant weight loss following surgery is not discoverable from our study.
However, given that improvements in skin changes were seen 10 to 36 months following surgery, when maximal weight loss is expected to be achieved (reflected in the average decrease in weight in the Post-Surgery group by 54.8 ± 20.9 kg), it may be that these improvements occur as a result of weight loss. Indeed, a study investigating the basis of CVI in obesity has shown that the decrease in femoral vein flow and increase in femoral vein diameter that is seen in obese individuals, is replicated consistently by increasing intra-abdominal pressure in lean adults [11]. This suggests that high intra-abdominal pressure being transmitted to lower limb veins may be a component of the venous hypertension (and consequent skin problems in the lower legs) that is seen in obesity. Following on from this is that weight loss occurring after bariatric surgery leads to decreased intra-abdominal pressure, leading to decreased venous hypertension in the lower limb by improving femoral vein outflow, and the improvement in lower leg skin problems. Other studies investigating the link between obesity and lower limb symptoms have shown that obesity itself, separate from its link to CVI, plays a major role in the development of lower limb ulceration [12]. In addition, a reduction in calf muscle pump function, and popliteal vein compression, particularly in the setting of obesity, have also been demonstrated to contribute to lower limb skin changes [13,14]. These studies support the postulated mechanism that a reduction in obesity following bariatric surgery may directly affect lower limb skin changes.
Because bariatric surgery potentially deals with the underlying pathology of skin changes, it is expected that it prevents recurrence of the skin problems-a definite benefit as they are often difficult to treat by conventional means using dressings, medications and compression stockings, and often recur. However, there is no current literature documenting the long- term effect of bariatric surgery on recurrence of lower leg skin problems.
The prevalence of varicose veins appears to be increased in the Post-Surgery group, compared to the Obesity Clinic group. This was an unexpected finding; given that the underlying presumed venous insufficiency that is potentially improved by bariatric surgery should in theory also decrease the prevalence of varicose veins, which is caused by the same underlying process. It may be that varicose veins that are already present become more visible as the patient loses weight. One way to investigate this further would be to perform duplex ultrasounds on the legs of obese individuals, to determine the sonographic prevalence of varicose veins in these individuals as compared to self-reporting by patients.
Ongoing treatment for obesity-related skin problems are a burden on the health system. The lower prevalence of those receiving treatment in the Post-Surgery group in our study, coupled with the observation that bariatric surgery seems to improve skin changes, suggests that in the long run, bariatric surgery may prove to be the cost-effective way to treat lower limb skin changes that occur with obesity.
One of the limitations of the study is the retrospective component of the Pre-Surgery Recall group, potentially leading to recall bias, as patients were asked to recall symptoms from up to 36 months prior to the study. It may be that patients in the Pre-Surgery Recall group were recalling ever having had an ulcer in the years leading up to surgery, compared to the Obesity Clinic group that had to state if they were currently having an ulcer at the time of filling out the questionnaire (not taking into account if they had an ulcer in the past). This may explain the differences in the prevalence of some of the individual symptoms between the Pre-Surgery Recall and the Obesity Clinic groups. Alternatively, selection bias may account for the differences, reflecting the greater likelihood of patients with more severe obesity-related symptoms being selected for surgery. Another limitation is the modest number of participants in the study. Even so, the differences were marked and achieved statistical significance.
This study investigated the prevalence of self-reported skin problems in the legs of morbidly obese patients and the impact of bariatric surgery. It confirmed that morbidly obese people have a high prevalence of skin problems in their lower legs. Bariatric surgery significantly lowers the prevalence of these symptoms. These findings result in the conclusion that bariatric surgery helps in the resolution of lower leg skin problems, particularly ulcers, in morbidly obese people, possibly by improving chronic venous insufficiency by reduction in intra-abdominal pressure and body weight.
References
- Lane RJ, Cuzzilla ML, Harris RA, Phillips MN (2009) Popliteal vein compression syndrome: obesity, venous disease and the popliteal connection. See comment in PubMed Commons below Phlebology 24: 201-207.
- Jawien A (2003) The influence of environmental factors in chronic venous insufficiency. See comment in PubMed Commons below Angiology 54 Suppl 1: S19-31.
- van Rij AM, De Alwis CS, Jiang P, Christie RA, Hill GB, et al. (2008) Obesity and impaired venous function. See comment in PubMed Commons below Eur J Vasc Endovasc Surg 35: 739-744.
- Willenberg T, Schumacher A, Amann-Vesti B, Jacomella V, Thalhammer C, et al. (2010) Impact of obesity on venous hemodynamics of the lower limbs. See comment in PubMed Commons below J Vasc Surg 52: 664-668.
- Robertson L, Lee AJ, Gallagher K, Carmichael SJ, Evans CJ, et al. (2009) Risk factors for chronic ulceration in patients with varicose veins: a case control study. See comment in PubMed Commons below J Vasc Surg 49: 1490-1498.
- World Health Organization (2014) Obesity and overweight.
- Buchwald H, Avidor Y, Braunwald E, Jensen MD, Pories W, et al. (2004) Bariatric surgery: a systematic review and meta-analysis. See comment in PubMed Commons below JAMA 292: 1724-1737.
- Picot J, Jones J, Colquitt JL, Gospodarevskaya E, Loveman E, et al. (2009) The clinical effectiveness and cost-effectiveness of bariatric (weight loss) surgery for obesity: a systematic review and economic evaluation. See comment in PubMed Commons below Health Technol Assess 13: 1-190, 215-357, iii-iv.
- Keating CL, Dixon JB, Moodie ML, Peeters A, Playfair J, et al. (2009) Cost-efficacy of surgically induced weight loss for the management of type 2 diabetes: a randomized controlled trial. See comment in PubMed Commons below Diabetes Care 32: 580-584.
- Abbade LP, Lastória S, Rollo Hde A (2011) Venous ulcer: clinical characteristics and risk factors. See comment in PubMed Commons below Int J Dermatol 50: 405-411.
- Willenberg T, Clemens R, Haegeli LM, Amann-Vesti B, Baumgartner I, et al. (2011) The influence of abdominal pressure on lower extremity venous pressure and hemodynamics: A human in-vivo model simulating the effect of abdominal obesity. Eur J Vasc Endovasc Surg 41: 849-855.
- Padberg F Jr, Cerveira JJ, Lal BK, Pappas PJ, Varma S, et al. (2003) Does severe venous insufficiency have a different etiology in the morbidly obese? Is it venous? See comment in PubMed Commons below J Vasc Surg 37: 79-85.
- Araki CT, Back TL, Padberg FT, Thompson PN, Jamil Z, et al. (1994) The significance of calf muscle pump function in venous ulceration. See comment in PubMed Commons below J Vasc Surg 20: 872-877.
- Lane RJ, Cuzzilla ML, Harris RA, Phillips MN (2009) Popliteal vein compression syndrome: obesity, venous disease and the popliteal connection. See comment in PubMed Commons below Phlebology 24: 201-207.
Tables and Figures at a glance
| Table 1 | Table 2 |
Figures at a glance
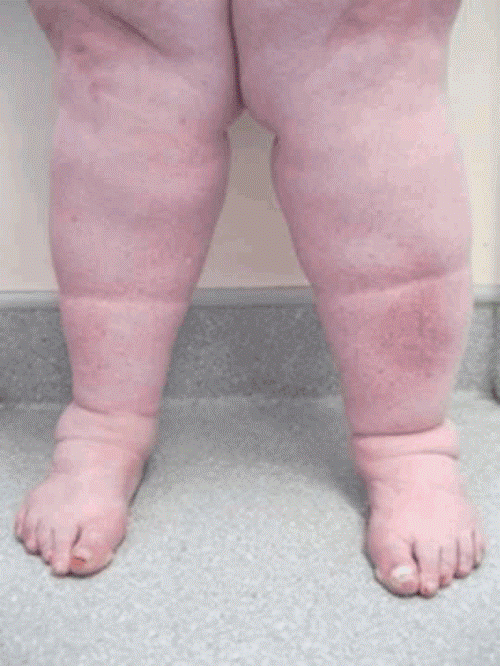 |
| Figure 1 |
Relevant Topics
- Android Obesity
- Anti Obesity Medication
- Bariatric Surgery
- Best Ways to Lose Weight
- Body Mass Index (BMI)
- Child Obesity Statistics
- Comorbidities of Obesity
- Diabetes and Obesity
- Diabetic Diet
- Diet
- Etiology of Obesity
- Exogenous Obesity
- Fat Burning Foods
- Gastric By-pass Surgery
- Genetics of Obesity
- Global Obesity Statistics
- Gynoid Obesity
- Junk Food and Childhood Obesity
- Obesity
- Obesity and Cancer
- Obesity and Nutrition
- Obesity and Sleep Apnea
- Obesity Complications
- Obesity in Pregnancy
- Obesity in United States
- Visceral Obesity
- Weight Loss
- Weight Loss Clinics
- Weight Loss Supplements
- Weight Management Programs
Recommended Journals
Article Tools
Article Usage
- Total views: 30179
- [From(publication date):
December-2014 - Apr 03, 2025] - Breakdown by view type
- HTML page views : 25610
- PDF downloads : 4569
