Case Report Open Access
Rupture of Uterus in Mid Trimester of Pregnancy: A Case Series & Review of Literature
| Chanderdeep Sharma*, Manupriya Sharma, Anjali Soni, P K Soni, Amit Gupta and Suresh Verma | |
| Dr. Rajendra Prasad Government Medical College, Tanda, Kangra, Himachal Pradesh, India | |
| Corresponding Author : | Dr Chanderdeep Sharma Assistant Professor (OBG) Dr. Rajendra Prasad Government Medical College Tanda, Kangra, Shimla Himachal Pradesh University, India Tel: 91-9218925471 E-mail: cdsharma2006@gmail.com |
| Received April 27, 2015; Accepted May 13, 2015; Published May 16, 2015 | |
| Citation: Sharma C, Sharma M, Soni A, Soni PK, Gupta A, et al. (2015) Rupture of Uterus in Mid Trimester of Pregnancy: A Case Series & Review of Literature. J Preg Child Health 2:163. doi: 10.4172/2376-127X.1000163 | |
| Copyright: © 2015 Sharma C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Pregnancy and Child Health
Abstract
With the increasing rates of cesarean section (CS) worldwide, pregnant women with previous CS are also rising at an alarming rate. This is leading to increase in previously rare complications of pregnancy e.g. cesarean scar pregnancy, placenta accreta and rupture uterus. One such complication is mid trimester rupture of uterus, which previously used to be a rare possibility. Now a day’s more and more pregnant women are presenting in shock in mid trimester of pregnancy. Hence, this case series is being reported to highlight this complication of pregnancy and to remind managing obstetricians and sonologists regarding these rare possibilities which should be kept in mind while doing routine sonographic assessment of pregnant women, so as to prevent catastrophe of rupture uterus.
| Keywords |
| Rupture uterus; Mid trimester; Cesarean scar pregnancy; Rudimentary horn rupture; Septic abortion |
| Introduction |
| The rates of cesarean section (CS) are increasing at an alarming rate worldwide [1]. This is leading to increasing occurrence of previously very rare complications of labor e.g. uterine rupture or morbid adherent placenta. Even though there is tremendous importance on rupture uterus or scar dehiscence during labor, there is little focus on mid trimester rupture of uterus (in second trimester of pregnancy). With exponential increase in number of pregnant women with previous CS [1,2], this rare but potentially catastrophic complication of pregnancy (mid trimester rupture of uterus) is further going to increase in near future. We hereby report three cases of mid trimester rupture of pregnant uterus (Table 1). |
| Case 1 |
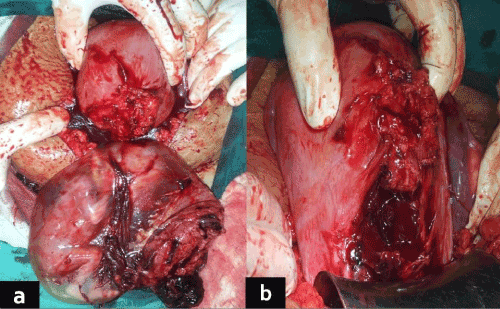
| A 26-year-old pregnant woman, (gravida 2, para 1), presented to emergency room (ER) at 17 weeks of gestation, with severe abdominal pain since last 2 hours. Her previous delivery was by emergency cesarean section (CS). This pregnancy was uneventful till date. On general examination, she had severe pallor, her pulse rate was 126 beats per minute (bpm) and blood pressure (BP) was 96/66 mm of Hg. On abdominal examination severe guarding was present; contour of uterus could not be made out. On pelvic examination, cervical os was closed; there was no bleeding per vaginum. Height of uterus could not be made out, even by bimanual examination. Emergency investigations revealed hemoglobin (Hb) of 4.8 g/dl. Emergency ultrasonography revealed hemoperitoneum with missed abortion and fetal lying outside uterus. Immediately decision of emergency laparotomy was made. Intraoperatively she had two liters of hemoperitoneum. There was rupture of previous CS scar and dead fetus along with entire amniotic sac was lying in the peritoneal cavity (Figure 1). So, a diagnosis of cesarean scar pregnancy followed by uterine rupture was made. Dead fetus was removed from the maternal abdomen followed by repair of CS scar. She received four units of blood transfusion (packed RBC’s) and one unit each of fresh frozen plasma (FFP) & platelet concentrate (PC). Her post-operative recovery was unremarkable and she was discharged in healthy condition on day 6 post-operative. |
| Case 2 |
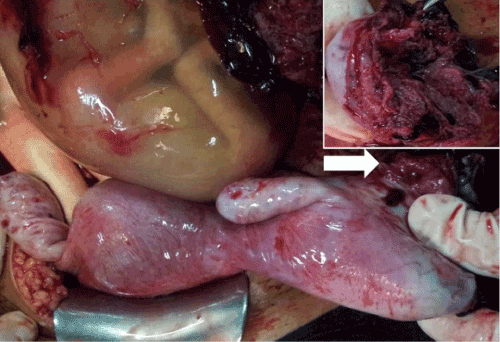
| A 34-year-old pregnant woman, (gravid 4, para 3) presented to outpatient department at 19 weeks of gestation, with severe abdominal pain since last few hours. She had all three previous normal vaginal deliveries. On examination she was in shock; pulse rate 140 bpm, systolic BP 84 mm of Hg and severe pallor. Her abdomen was tense with guarding. On pelvic examination, cervical os was closed. There was no bleeding per vaginum. Immediately resuscitative measures were started and emergency investigations were sent. Her hemoglobin was 3 g/dl and ultrasonography revealed massive hemoperitoneum with missed abortion. She was shifted to OT, where intra-operatively she was found to have three liters of hemoperitoneum and rupture of non-communicating rudimentary horn of uterus (Figure 2). After thorough peritoneal toileting and removal of dead fetus from peritoneum, surgical excision of non-communicating rudimentary horn of uterus was done. She received six units of packed RBC’s, two units of FFP & PC’s each. She was subsequently discharged on day 7 post-operatively in healthy condition. |
| Case 3 |
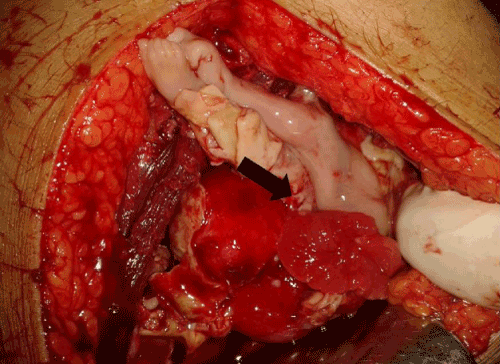
| A 21-year-old pregnant woman, (gravid 2, para1) at 17 weeks 4 days of gestation presented to emergency room in shock. She had a previous normal vaginal delivery. Her pulse rate was 162 bpm, respiratory rate was 28 bpm and systolic BP was 60 mm of Hg. Immediately resuscitative measures were started and simultaneously investigations were sent. She had hemoglobin of 4 g/dL. Even after thorough probing, no history of any intervention was given. On examination, abdomen was tense; there was severe guarding and rigidity. Supine X-ray revealed air under the right dome of diaphragm. Urgent sonography revealed massive hemoperitoneum with fetal death. Patient was rushed to operation theatre with a probable diagnosis of rupture uterus with perforation of gut. Intra-operatively, there was massive hemoperitoneum (4 liters) was present; there was rupture of the fundus of uterus with fetal legs protruding into the peritoneal cavity (Figure 3). Sigmoid colon was perforated with fecal matter lying in the peritoneal cavity. Repair of the colonic perforation (with colostomy) with repair of uterine perforation and delivery of dead fetus was done. Subsequently relatives confirmed the history of septic induced abortion. Patient received 5 units of blood transfusions. She was fortunate to have uneventful recovery. |
| Discussion |
| Rupture of pregnant uterus is a catastrophic event with severe fetal and maternal morbidity and mortality. Massive increase in rates of CS, have made this rare complication a relatively common phenomenon these days. Majority of focus now a days is on “in labor” scar dehiscence or uterus rupture. However, pre-labor and even mid trimester rupture of uterus is also rising due to exponential increase in number of women with previous CS [1]. There is paucity of available literature and standard guidelines on this complication. Majority of literature has only case reports to derive conclusions regarding management of this uncommon but potentially catastrophic complication. Some of the common causes of mid trimester uterine rupture are cesarean scar pregnancy, ruptured rudimentary horn pregnancy, medical termination of pregnancy with abortifacients (e.g. mifepristone or misoprostol; especially in case of pregnancy after previous CS) and illegal abortion. Usually the diagnosis and hence management of this complication is late (after rupture has occurred and patient is in shock), especially in developing countries with paucity of resources and inadequately trained manpower to diagnose these un-common presentations (cesarean scar pregnancy or rudimentary horn pregnancy). |
| Cesarean scar pregnancy CSP refers to implantation of the gestational sac in the scar of the previous cesarean section [1]. It is a relatively rare complication (with an estimated incidence of 1 in 2,500 CS) [1] but with a very high complication rate in terms of severe maternal & fetal morbidity & mortality. Early diagnosis of cesarean scar pregnancy has been found to be beneficial for conservative management. Localization of the chorionic sac in the depth of the niche (ultrasonic image of filling defect in the cesarean scar created after the healing process), is the mainstay in early diagnosis of cesarean scar pregnancy [3]. However, in 13.6% of the cases the early diagnosis is missed and these patients present in emergency with catastrophic outcomes [4] of all the available investigations, high frequency transvaginal ultrasound is the best diagnostic tool [1,3]. |
| Diagnostic criteria [4] for Cesarean Scar pregnancy are; (positive pregnancy test with) |
| • Empty uterine and endocervical canal. |
| • Placenta and/or a gestational sac embedded in the cesarean scar |
| • Gestational sac filling the niche of the scar at early gestation (< 8 weeks) |
| • Thin (1-3 mm) or absent myometrial layer between the gestational sac & bladder |
| • Presence of embryonic/fetal pole and/or yolk sac with or without heart activity. |
| • Presence of a prominent vascular pattern at or in the area of a cesarean scar |
| Due to the lack of definite management-guidelines various treatment options have been tried with optimal success [5-10]. These options are intra muscular methotrexate, hysteroscopic excision, ultrasound guided intra gestational injection of methotrexate or potassium chloride, uterine artery embolization with & without dilatation & curettage and a combination of the above mentioned procedures [1,4-10]. These conservative management options have been associated with complications like severe hemorrhage (more than 2 liters), hemoperitoneum, shock, or uterine rupture. Till date the least complication rate has been observed with local intra-gestational injection of methotrexate or potassium chloride under ultrasonic guidance (9.6%) in comparison to very high complication rates with methotrexate injection alone (62.1%) or dilatation & curettage (61.9%) [1]. |
| However, uterine rupture has to be treated with life-saving emergency laparotomy with either repair of uterine rent or emergency hysterectomy. Uterine artery embolization, if available, can be used as an adjunct to minimize the blood loss [1]. As was seen in case 1, where the patient had an un-complicated previous cesarean delivery and was routinely managed in this pregnancy. However, it led to cesarean scar pregnancy and uterine rupture, thereby posing serious maternal morbidity and fetal mortality. |
| Pregnancy in a rudimentary horn of uterus is an uncommon occurrence. Its exact incidence is unknown. More than 300 cases have been reported till date [11]. Rupture of rudimentary horn is associated with very high rates of fetal mortality and severe maternal morbidity. However maternal mortality is low (0.5%) [12-14]. The diagnosis of pregnancy in rudimentary horn before rupture of uterus is mainly by ultrasonography. But the sensitivity of ultrasound to detect prerupture rudimentary horn pregnancy is very poor (30%) [13,14], due to rare occurrence and poor knowledge of radiologists regarding this complication. |
| If early diagnosis before rupture is done, these women can be managed laparoscopically by excision of the horn, pregnancy, and the ipsilateral fallopian tube [14]. Diagnostic criteria on the basis of ultrasonography [15] for rudimentary horn pregnancy are; |
| • pseudo pattern of an asymmetrical bicornuate uterus |
| • absent visual continuity tissue surrounding the gestation sac and the uterine cervix |
| • the presence of myometrial tissue surrounding the gestation sac |
| In case of any doubt three-dimensional ultrasound or magnetic resonance imaging should be done to avoid the potential complications. The possibility of iatrogenic interference (whether legal or illegal) should always be kept in mind while dealing with pregnant women in shock in mid trimester of pregnancy (whether or not a straight forward history is present). History of procedures like dilatation and curettage, hysteroscopy, endometrial ablation and insertion of intrauterine contraceptive devices predispose to rupture uterus [16,17]. Dilatation and curettage is a commonly performed procedure and is considered to be relatively safe with low overall complication rate of 0.7 %, however its use is limited to first trimester and that too less than 10 weeks of gestation. But in many illegal settings, it is still being done as a last resort for abortion, especially in poor population with social stigma of pregnancy in unmarried women with limited access to health care facilities. According to World health Organization (WHO) estimates there is a case fatality rate of 250-500 deaths per 100,000 illegal abortion procedures [18]. Some factors like instillation of saline or prostaglandins, advanced gestational age have been associated with a higher complication rate. Extensive use of mifepristone and misoprostol has made abortion fairly safe, but still possibility of rupture uterus is always there (whether these abortifacients have been used or not), especially in women with a history of previous CS (even though rupture uterus have been reported in unscarred uterus with use of these agents). |
| Diagnosis of iatrogenic mid trimester rupture uterus is usually clinical with clear history of surgical interference. However, in cases of illegal abortions such a history is not straight forward (as was seen in index case) and ultrasonography indirectly helps in diagnosis with visualization of bowel loops in myometrial or endometrial cavity or demonstration of extra-uterine fetal parts in a pregnant female. Sometimes even the site of rupture may be identified as a hypoechoic or anechoic transmural defect in myometrium extending to endometrium with presence of extrauterine fliud [19]. Associated perforation of unprepared large gut as seen in the index case (case 3; sigmoid colon perforation) can be easily diagnosed clinically by signs and symptoms of peritonitis. |
| The main presentation feature of women with mid trimester rupture uterus is “shock out of proportion of visible blood loss”. All these women required urgent resuscitative measures and urgent laparotomy which is life-saving. “A history of previous CS” is a very important point in history as it may point towards the possibility of cesarean scar pregnancy/placenta accreta. Nonetheless, other obstetric causes of shock e.g. ruptured rudimentary horn, ectopic pregnancy, trauma, and perforation/rupture uterus due to surgical interference should also be kept in differential diagnosis. Any signs symptoms of peritonitis may point towards surgical evacuation of uterus with concomitant perforation uterus with gut perforation. However, mainstay of diagnosis and management in these cases is “explorative laparotomy” and time should not be wasted for making a definite diagnosis as any delay may seriously hamper the chances of maternal survival. |
| “Prevention is better than cure,” this idiom holds true in this particular complication of pregnancy, where an early diagnosis and management of hemodynamically stable patient is much better than explorative laparotomy for rupture uterus. |
| Conclusion |
| Mid trimester rupture uterus is an uncommon diagnosis and is usually made when pregnant women presents in shock in the second trimester of pregnancy. However, efforts should be made to have an early diagnosis before rupture has actually occurred in order to avoid serious maternal morbidity and mortality. This is only possible if high index of suspicion is there and managing obstetricians and ultrasonologists/ radiologists are aware of these complications in pregnant women which are occurring with an increasing frequency in the present era. |
| Conflict of Interest |
| Authors’ state there is no conflict of interest with any individual or organization. |
References
- Timor-Tritsch IE Monteagudo A (2012) Unforeseen consequences of the increasing rate of cesarean deliveries: early placenta accreta and cesarean scar pregnancy. A review. Am J ObstetGynecol 207: 14-29.
- Litwicka K Greco E (2011) Caesarean scar pregnancy: a review of management options. CurrOpinObstetGynecol 23: 415-421.
- Monteagudo A Carreno C, Timor-Tritsch IE (2001) Saline infusion sonohysterography in nonpregnant women with previous cesarean delivery: the "niche" in the scar. J Ultrasound Med 20: 1105-1115.
- Timor-Tritsch IE Monteagudo A, Santos R, Tsymbal T, Pineda G, et al. (2012) The diagnosis, treatment, and follow-up of cesarean scar pregnancy. Am J ObstetGynecol 207: 44.
- Litwicka K Greco E (2011) Caesarean scar pregnancy: a review of management options. CurrOpinObstetGynecol 23: 415-421.
- Sadeghi H Rutherford T, Rackow BW, Campbell KH, Duzyj CM, et al. (2010) Cesarean scar ectopic pregnancy: case series and review of the literature. Am J Perinatol 27: 111-120.
- Kucera E Krepelka P, Krofta L, Feyereisl J (2007) [Cesarean scar ectopic pregnancy]. CeskaGynekol 72: 207-213.
- Fabunmi L Perks N (2002) Caesarean section scar ectopic pregnancy following postcoital contraception. J FamPlannReprod Health Care 28: 155-156.
- Tulpin L Morel O, Malartic C, Barranger E (2009) Conservative management of a Cesarean scar ectopic pregnancy: a case report. Cases J 2: 7794.
- Li SP Wang W, Tang XL, Wang Y (2004) Cesarean scar pregnancy: a case report. Chin Med J (Engl) 117: 316-317.
- Fitzmaurice LE Ehsanipoor RM, Porto M (2010) Rudimentary horn pregnancy with herniation into the main uterine cavity. Am J ObstetGynecol 202: e5-6.
- Nahum GG1 (2002) Rudimentary uterine horn pregnancy. The 20th-century worldwide experience of 588 cases. J Reprod Med 47: 151-163.
- Chopra S Keepanasseril A, Rohilla M, Bagga R, Kalra J, et al. (2009) Obstetric morbidity and the diagnostic dilemma in pregnancy in rudimentary horn: retrospective analysis. Arch GynecolObstet 280: 907-910.
- Jayasinghe Y Rane A, Stalewski H, Grover S (2005) The presentation and early diagnosis of the rudimentary uterine horn. ObstetGynecol 105: 1456-1467.
- A Tsafrir, N Rojansky HY, Sela JM, Gomori, M Nadjari (2005) “Rudimentary horn pregnancy: first-trimester prerupturesonographic diagnosis and confirmation by magnetic resonance imaging,”. Journal of Ultrasound in Medicine 24: 219–223.
- Caspi B, Rabinerson D, Appelman Z, Kaplan B (1996) Penetration of the bladder by a perforating intrauterine contraceptive device: a sonographic diagnosis. Ultrasound ObstetGynecol7:458-460.
- Irvin W Rice L, Taylor P, Andersen W, Schneider B (2003) Uterine perforation at the time of brachytherapy for carcinoma of the cervix. Gynecol Oncol 90: 113-122.
- Dragoman M, Sheldon WR, Qureshi Z, Blum J, Winikoff B, Ganatra B; WHO Multicountry Survey on Maternal Newborn Health Research Network. Overview of abortion cases with severe maternal outcomes in the WHO Multicountry Survey on Maternal and Newborn Health: a descriptive analysis. BJOG. 2014 Mar;121Suppl 1:25-31. doi: 10.1111/1471-0528.12689.
- Gakhal MS, Levy HM (2009) Sonographic diagnosis of extruded fetal parts from uterine perforation in the retroperitoneal pelvis after termination of intrauterine pregnancy that were occult on magnetic resonance imaging. J Ultrasound Med 28:1723-1727.
Tables and Figures at a glance
| Table 1 |
Figures at a glance
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 |
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 15080
- [From(publication date):
June-2015 - Jul 06, 2025] - Breakdown by view type
- HTML page views : 10372
- PDF downloads : 4708
