Review Article Open Access
Lumbar Spinal Instability: An Updated Rewiew
| Alessandra Splendiani*, Lucia Patriarca, Silvia Mariani, Ernesto Di Cesare and Massimo Gallucci | |
| Department of Radiology, University of L’Aquila, Ospedale Sm di Collemagio, I-167100, L’Aquila, Italy | |
| Corresponding Author : | Alessandra Splendiani Department of Biotechnological and Applied Clinical Sciences University of L’Aquila, I-167100, L’Aquila, Italy Tel: +393479902770 E-mail: alessandra.splendiani@cc.univaq.it |
| Received December 03, 2014; Accepted January 07, 2015; Published January 10, 2015 | |
| Citation: Splendiani A, Patriarca L, Mariani S, Cesare E, Gallucci M (2015) Lumbar Spinal Instability: An Updated Rewiew. OMICS J Radiol 4:178. doi: 10.4172/2167-7964.1000178 | |
| Copyright: ©2015 Splendiani A et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Radiology
Abstract
Supine Magnetic Resonance Imaging (MRI) is routinely used in the assessment of low- back pain and radiculopathy. However, imaging findings often correlate poorly with clinical findings. This is partly related to the positional dependence of spinal stenosis, which reflects dynamic changes in soft-tissue structures. Upright MRI in the flexed, extended, rotated, standing, and bending positions allows patients to reproduce the positions that bring about their symptoms. Assessment of the degree of spinal stability in the degenerate and postoperative lumbar spine is also possible and it offers many diagnostic opportunities. The aim of this rewiew is to present the findings concerning the spine instability using conventional and upright MRI.
| Keywords |
| Lumbar instability; Spinal MRI; Dynamic MRI; Degenerative spine |
| Introduction |
| According to the American Academy of Orthopaedic Surgeons, instability was defined as an abnormal response to applied loads, characterized by movement in the motion segment beyond normal constraints in 1989. Segmental instability has been defined as occurring in patients with low back problems and whose clinical status is unstable, with symptoms fluctuating between mild and severe symptoms in response to even minor provocations. The validity of these clinical definitions has not been demonstrated. Frymoyer et al defined segmental instability as “a condition where there is loss of spinal stiffness, such that normally tolerated external loads will result in pain” [1,2]. |
| Clinical criteria for lumbar spine instability have not yet been clearly defined [3]. Recurrent, acute episodes of low back pain produced by mechanical stresses have been considered to be indicative of instability . If a full return from the bent position fails because of a sudden attack of low back pain (ie, instability catch), if a patient is unable to get a raised, straightened leg to move down and suddenly drops the leg due to a sharp pain in the low back(ie, painful catch), and if a patient feels anxiety resulting from a sensation of collapse of the low back because of a sudden attack of back pain during movement (ie, apprehension), the patient fulfills the three criteria for instability described by Kotilainen and Valtonen. A loss of tone in the legs or in the low back and pelvic region (ie, giving away phenomenon) has also been observed in some patients with lumbar instability. However, these clinical criteria have not been rigorously evaluated. |
| Iguchi et al [4] measured sagittal segmental instability at L4/ L5 disc using three lateral radiographs at neutral, extension, and flexion position, was assessed by three variables: L4 anterior slip on L5 in neutral position (SN), sagittal translation (ST), and segmental angulation (SA) using the method basically described by White and Panjabi, which has only three landmarks for the measurement: the anterior edge and the posterior edge of upper endplate of L5, and the inferior posterior edge of L4. 447 patients, 268 men and 179 women, were included in this study and their age range varied from 10 to 86 years (mean ± SD: 53.0 ± 19.8) In all patients were performed MRI study to evaluate the disc height and grade of degeneration. The disc height showed an intimate relationship with age and instability, and furthermore the principal part of the instability factors changed across age decades: ≥ 10° angulation, ≥ 3 mm translation, and finally ≥ 3 mm slip. Combination of the ≥ 3 mm slip and the ≥ 3 mm translation were closely related to severe symptoms and considered to be critical for surgical indication [5,6]. |
| Maigne et al studied 42 patients with low back pain occurring immediately on sitting down and relieved on standing up. Comparing clinical, radiographic, and magnetic resonance data they found an important association between symptom and imaging signs of instability (100% specificity, 31% sensitivity) or severe anterior loss of disk space in flexion (87% specificity, 55% sensitivity) [7]. |
| MR imaging is generally considered to be the most valuable method to diagnose degenerative abnormalities of the spine, except for the vacuum phenomenon, and it is often considered the most useful modality for evaluation of myelopathy, radiculopathy, and low back pain requiring advanced imaging. Identification of patients with an increased chance of instability on MR images can be clinically relevant and can influence indications for flexion-extension radiography [6]. |
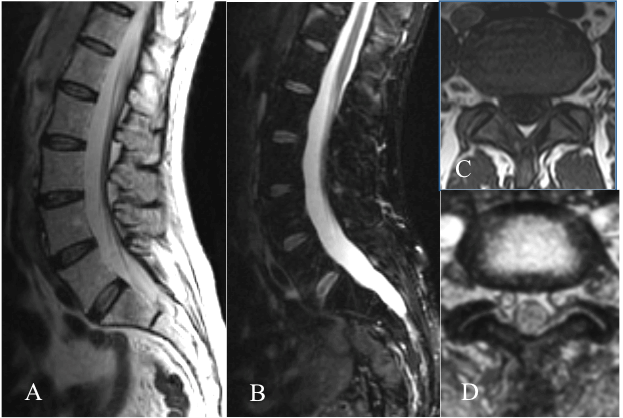
| The superior contrast resolution of MRI depicts the soft tissue anatomy of the spine better than plain films and CT. The spinal cord, nerve roots, cerebral spine fluid (CSF), vertebrae, discs, and ligaments can be exquisitely resolved and distinctly visualized (Figure 1) [8]. Thanks to technological improvements in MR equipment (fast gradient systems, parallel imaging, multielement phased-array coils), basic MR techniques including spin-echo (T1- and T2-weighted images), gradient-echo and fat saturation sequences are now characterized by high resolution and increased signal-to-noise ratio. In addition, many supplementary techniques have been introduced, e.g. steady-state sequences (like CISS or FIESTA), which provide excellent delineation of the outlines of disc herniations; MR myelography, a non-invasive technique that has replaced conventional CT myelographies; and post-contrast sequences, which are especially useful in post-operative studies [9,10]. |
| Axial GRE is typically used to assess degenerative disease in the cervical spine. Unlike SE and FSE sequences disc material (hyperintense on GRE) and osteophytes (hypointense), can be differentiated with GRE, regardless of flip angle. |
| Balanced steady state free procession (bSSFP) sequences also have an inherently high contrast between tissue and fluid. Moreover, compared with unbalanced steady state free procession (SSFP) sequences, bSSFP provides high baseline SNR. Thus, it provides an efficient alternative sequence for better detection of herniations, sequestrations or nerve root compression. Conversely, the gray/white matter contrast of conventional bSSFP is relatively poor [11]. |
| SE and FSE sequences provide good anatomic detail in spine imaging and are favored for the evaluation of spinal canal diameter and the detection of spinal cord abnormalities, with less susceptibility artifact from bone and improved contrast between gray and white matter structures within the cord, compared with GRE. Given the abundance of epidural fat within the lumbar spine and the relatively large disc spaces, FSE sequences are favored over GRE in lumbar spine imaging to assess focal disc protrusion and nerve root compression. However, the CSF adjacent to the cord, together with cord motion, often causes ghosting artifacts in conventional Cartesian imaging, expecially in FSE T2-weighted images [11,12]. |
| Additional sequences may be helpful in case of persistent unexplained symptoms, for more complex or specific question about anatomy or the influence of patient position on alignment and stenoses. Contrast- enanced T1-wheighted images with fat saturation can reveal facet joint pathology, spondylolysis, spinal degenerative/inflammatory changes and changes within the paraspinal muscles, which are not always evident on conventional imaging [14,15]. Recently there have been attempts to apply advanced supplementary techniques, such as diffusion-weighted imaging (DWI) and diffusion tensor imaging (DTI), functional (motion) imaging, MR spectroscopy and functional MR (fMRI) [13,14]. |
| Degenerative diskogenic vertebral changes can be noted on vertebral endplates (Modic types 1–3). There are degenerative changes such as intervertebral osteochondrosis that are considered pathologic and not due to normal aging, including desiccation and narrowing of the disc, gas in the disc, disc bulging, radial annular tears, posterior osteophytes, endplate sclerosis and erosions, and chronic bone marrow changes adjacent to the disc interspaces. Radial annular tears are failures of multiple annular layers. They are bright on T2-weighted images and may enhance. Modic type 1 corresponds to increased vascularity in the juxta-endplate vertebra. Its MRI appearance reflects increased water content: dark on T1-weighted images and bright on T2-weighted image. Modic type 2 represents increased fatty marrow: bright on T1-weighted and dark on fat-suppressed T2-weighted FSE images. Modic type 3 denotes sclerotic changes: dark on both T1- and T2-weighted images. Posterior osteophytes are also dark on both T1- and T2-weighted images and can narrow the spinal canal and neural foramina. Extensive gas in the disc (vacuum disc) can be seen on plain films and CT, and sometimes on MRI [12]. |
| The association of vertebral instability and changes in the bone marrow adjacent to the endplates has been discussed, but without consistent results . Modic et al stated that the clinical importance of these changes in the bone marrow is unknown. Lang et al observed bone marrow changes adjacent to the endplates in postoperative instability, but no statistically significant correlation exists between segmental instability and abnormalities of the bone marrow adjacent to the endplates in patients without spinal fusion, as resulted from a study of Bram et al in 1998. Conversely, Bram et al found a significant association between radiographic instability and traction spurs and between radiographic instability and annular tears . In their study of patients with chronic low back pain, Aprill and Bogduk first described annular tears as a high-signal intensity dot on sagittal T2-weighted images in 1992. |
| Therefore, flexion-extension radiographs should be considered in patients with annular tears or traction spurs. Unfortunately, additional studies supporting this conclusion are necessary before it can be generally accepted. A high-signal-intensity zone in the posterior annulus fibrosus on sagittal T2-weighted images has been found much too frequently in asymptomatic subjects to be considered a reliable independent diagnostic indicator. |
| Spondylolysis can be defined as a defect in the pars interarticularis of the vertebral arch. This defect is seen relatively often in radiographic studies and may either occur asymptomatically or be associated with significant low back pain (LBP). Spondylolysis and spondylolisthesis, a related condition defined by forward displacement of one vertebral body over the subjacent one, were classified by Wiltse et al in 1976 as follows: Type I: dysplastic: congenital abnormalities of L5 or the upper sacrum allow anterior displacement of L5 on the sacrum. Type II: isthmic: a lesion in the pars interarticularis occurs. This is subclassified as [a] lytic, representing a fatigue fracture of the pars, [b] elongated but intact pars, and [c] acute fracture. Type III: degenerative, secondary to long standing intersegmental instability with associated remodelling of the articular processes. Type IV: traumatic, acute fractures in vertebral arch other than the pars. Type V: pathological, due to generalised or focal bone disease affecting the vertebral arch. |
| Studies from the radiology literature report that MRI has a sensitivity of up to 86 %, a specificity of 82 %, a positive predictive value of 18 %, and a negative predictive value of 99 % in the diagnosis of spondylolysis. However, recent studies show that 64% of spondylolysis in symptomatic patients referred for pediatric orthopaedic surgeon if MRI was performed alone [15]. |
| Spondylolisthesis is a debilitating chronic pathology, which generally begins with degeneration of the intervertebral discs and the facet joints, causing a narrowing of the vertebral canal and the neural foramen. A fundamental contribution to the study of this problem is provided by CT and MRI; in particular the latter enables a high degree of spatial and contrast resolution, and shows a precise evaluation of intervertebral discs, vertebrae, ligaments, spinal canal and intervertebral foramima. Despite the unquestionable diagnostic accuracy of these methods for morphological evaluation of these anatomical structures, when diagnosing foraminal stenosis, the number of false negatives is considerable, as shown in literature. Various studies conducted with CT and MRI on cadaveric experimental models underline the importance of the weight loading when examining the foramen. By subjecting in vitro cadaveric lumbar segments to movements of axial rotation, extension, bending and lateral curvature, a compression of the spinal nerve was observed, not detected by examinations without application of the weight [16-19] (Figures 1 and 2). |
| Degenerative disk disease and facet joint osteoarthritis affect the stability of the motion segment. However, the exact relationship between degenerative disk disease, facet joint osteoarthritis, and vertebral instability on MR imaging has not been defined. Fujiwara et al. also compared MR imaging and functional radiography of the lumbar spine to examine the relationship among segmental instability, disk degeneration, and facet joint osteoarthritis in patients with low back pain; they reported that an anterior translation of 3 mm or greater was positively associated with disk degeneration and facet joint osteoarthritis [1]. |
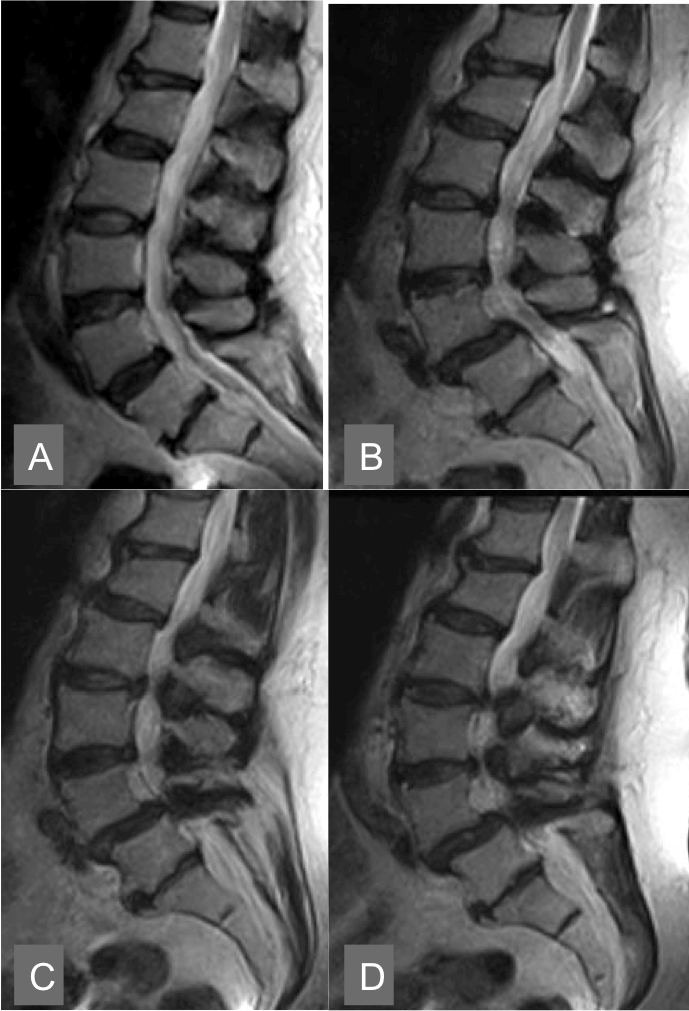
| Recently Splendiani et al reported a study which suggests that in some patients the pathogenesis of radicular pain is the result of a dynamic stenosis of the foramen caused by physiological load. They demonstrate that the association between disk pathology and facet osteoartrosis can determine foraminal occult stenosis. Supine imaging may not correctly represent the degree and the clinical revelance of a foraminal stenosis (Figure 3) [20]. |
| Although the lumbar spine undergoes large compression loads during normal activities, MRI imaging is routinely performed in supine and, only after, in upright position. Advances in MR techniques have made possible the development of open MRI systems, which provide the possibility to investigate spinal kinematics and vertebral instability. Early studies were limited to assessing spinal kinematics by imaging the patient in the supine position in combination with several different axial loading MRI– compatible devices and not truly reflect postural spinal changes related to muscle tone, loads on the lumbar spine that increase in a caudal direction rather than being uniform at each spinal level, and the effects of core muscle activation on the spine [21]. |
| The technological advancement of open MRI equipment with low-and medium-intensity magnetic field, greater gradient homogeneity, and faster sequences resulted in a significant improvement in Signal Noise Ratio (SNR) in spatial and contrast resolution and therefore image quality. Some MRI equipment are capable of obtaining images of the spine in orthostatic position, which could better show pathological conditions sometimes “missed” in supine position. These devices, all characterized by being open, also have the advantage of eliminating the patient’s feeling of claustrophobia, which sometimes limits the execution of diagnostic examination. Some publications in literature involve studying the lumbar spine using MRI equipment with the patient in the upright position, to evaluate the variations of physiological and pathological parameters of the lumbosacral spine in patients with acute and chronic low back pain [22-26]. |
| Weishaupt et al [27] evaluated thirty patients with chronic low back pain unresponsive to nonsurgical treatment and with disk abnormalities but without compression of neural structures at conventional (supine) MR imaging. Positional pain differences were related to position-dependent changes in foraminal size. Positional MR imaging demonstrated minor neural compromise more frequently than conventional MR imaging, but no convincing signs of canal or foraminal encroachments were found. |
| Wildermuth et al in 1998 compared measurements of the sagittal diameter of the lumbar dural sac obtained at positional Magnetic Resonance (MR) imaging and at functional myelography and assessed the influence of various body positions on the dural sac and the intervertebral foramina in 30 consecutive patients with combined low back pain and sciatica, who were examined in the supine, upright flexion, and upright extension positions with an open MRI equipment. They found that quantitative assessment of sagittal dural sac diameters is comparable between lumbar myelography and positional MR imaging and concluded that only small changes in the sagittal diameter of the dural sac and foraminal size can be expected between various body positions, and the information gained in addition to that from standard MR imaging is limited. |
| The evaluations of physiological and biomechanical elements showed that for each considered parameter, there are significant and meaningful differences depending on supine or upright position and sometimes even on gender; careful analysis of an MRI should therefore be performed according to these data interpreting subsequent pathological findings. Reduced lumbosacral and increased lordosis angle depend on activation of postural effects of body weight mediated by abdominal and paraspinal muscles. In standing position, the lumbosacral angle decreases in relation to verticality of the spine, which is necessary to support the increase in weight, whereas the increase in lordosis angle reflects compensation by muscle contracture. The reduction of intervertebral disc height was highly significant (p = 0.000083), undoubtedly due to body weight and muscle activation [8,11]. In particular, the reduction of disc height affects the posterior portion,whereas anteriorly, there was a slight increase, with major changes at L2–L3 and L3–L4 [23]. Observed variations in the lordosis and lumbosacral angle values confirm the already known physiological changes produced by the transition from supine to orthostatic position. |
| Imaging in the supine position and with non- dynamic methods can only identify indirect radiological signs of instability (i.e., degenerative changes of the disc, ligaments, and facet joints) and some direct signs (malalignment of the vertebral bodies). Upright and positional MRI can demonstrate changes in intersegmental motion that may correlate with clinical symptoms of Low Back Pain and neurogenic claudication. As yet, however, no published studies have dealt with this topic. |
| Instability can be considered as part of the normal degenerative process of the lumbar spine, which has three phases. Initially, there is abnormal motion of the spinal segment (disc, adjacent vertebrae, ligaments, facet joints) and pathological signs of degeneration are minimal; this stage being termed ‘‘spinal dysfunction’’. The signs of relative spinal motion (e.g., translation and sagittal rotation of the vertebral bodies with respect to each other) can be uncover with upright/positional MRI. |
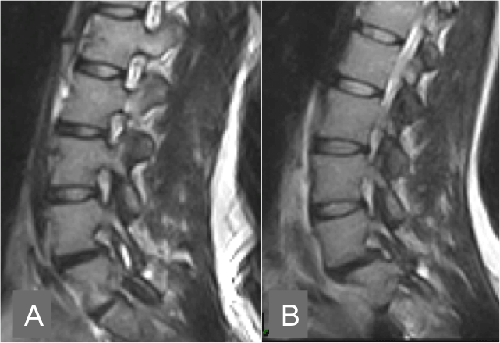
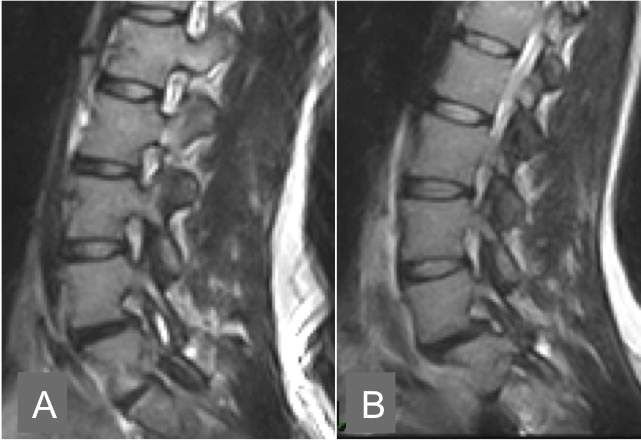
| During the second or ‘‘instability phase’’, signs of degeneration are more prominent and there is increased and abnormal intersegmental movement. Instability can be demonstrated as relative hypermobility at the spinal motion segment compared with adjacent motion segments on positional MRI (Figure 2). Excess extension can in turn increase the degree of foraminal, central and lateral recess stenosis, which may correlate with increased levels of pain. Instability of a degenerative or isthmic spondylolisthesis can increase central or foramina stenosis (Figure 3 and 4). The disc below a degenerate spinal level can be susceptible to degeneration and disk herniation changes in size under phisiological load (Figure 5). In the post-operative spine, damage to the paraspinal musculature and ligaments, and reduced motion at levels of fusion together with increased motion at the adjacent levels contribute to instability [21]. |
| As degeneration progresses, fibrosis and osteophytosis result in restabilization and consequential reduction in movement (third phase). This ‘‘restabilization phase’’ can be difficult to distinguish from the instability phase without positional imaging an important consideration if surgery is being contemplated. How often and when this distinction needs to be made remains to be determined. In the case of degenerative and isthmic spondylolisthesis, most appear stable, with no significant positional change in either angular rotation or horizontal translation [22-30]. As the degree of degenerative disc disease increases, the amount of angular rotation from the supine to the erect position significantly increases, with maximal rotation occurring at a normal level below the slip [25]. |
| Although the lower field strength of the open MRI equipment used for dynamic study results in a reduced signal to noise ratio, and thus, overall reduced image quality compared with high- field magnets, many authors suggest that image quality in the standing position can detect changes in intersegmental motion and correlate it with symptom. These aspects confirms the high sensitivity in assessing the lumbar spine under load conditions in the clinical suspicion of lumbar canal stenosis and nerve root compression [26-29]. Limitations of these study are mainly due to two factors: in the upright position, patients with acute low back pain may find it difficult to maintain the immobility necessary for the duration of the imaging acquisition with a duration of at least 4 min for each sequence. A second and equally important negative factor is the difficulty sometimes encountered in evaluating the most lateral areas of the spine, such as foramen and lateral recesses. |
| The images with the patient in the supine position may incorrectly represent the degree and clinical relevance of the foraminal stenosis. The dynamic imaging techniques may increase our ability to localize the original site of nerve root compression in patients suffering from LBP or radiculopathic pain. Therefore, the dedicated MR unit is offered as an instrument able to provide useful dynamic studies to obtain correct diagnoses. The rapid and prompt diagnostic framework on site and characteristics of the foraminal stenosis may provide useful guidelines for correct treatment procedures. Conservative medical treatment may prove effective in the initial phases in which a return of the biomechanical load limits the effects of compression over time. Surgical treatment should be performed on patients with debilitating and progressive pain or neurological dysfunctions. More recently, micro-invasive percutaneous approaches have been proposed which could make use of the anatomical and functional detail proposed, both in pre and post treatment testing, contributing to a more in-depth understanding of the phenomena at the base of such a widespread pathology with such high social costs. |
| More recently precutaneus minimal invasive approach has been also proposed. Therefore, since the early diagnosis and treatment of foraminal stenosis may prevent intractable pain and the permanent neurologic sequelae, MR dedicated unit able to perform orthostatic studies can be useful to achieve the correct diagnosis [30]. |
| Conclusion |
| In conclusion, supine MRI remains the technique of choice for detecting lumbar spinal instability associated with acute and chronic low back pain. However, in about one of three cases, conventional MRI performed in the supine position is unable to answer to clinical question . In cases where conventional MRI shows no evidence of cauda equina or lumbar nerve root compression in the setting of convincing clinical symptoms that warrant surgical intervention, reimaging in the upright position, with the addition of flexion and extension, is recommended. |
References |
|
Figures at a glance
 |
 |
 |
 |
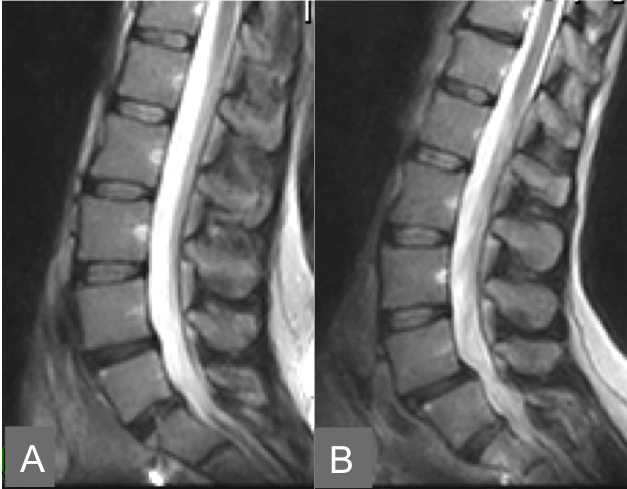 |
| Figure 1 | Figure 2 | Figure 3 | Figure 4 | Figure 5 |
Relevant Topics
- Abdominal Radiology
- AI in Radiology
- Breast Imaging
- Cardiovascular Radiology
- Chest Radiology
- Clinical Radiology
- CT Imaging
- Diagnostic Radiology
- Emergency Radiology
- Fluoroscopy Radiology
- General Radiology
- Genitourinary Radiology
- Interventional Radiology Techniques
- Mammography
- Minimal Invasive surgery
- Musculoskeletal Radiology
- Neuroradiology
- Neuroradiology Advances
- Oral and Maxillofacial Radiology
- Radiography
- Radiology Imaging
- Surgical Radiology
- Tele Radiology
- Therapeutic Radiology
Recommended Journals
Article Tools
Article Usage
- Total views: 22581
- [From(publication date):
February-2015 - Jul 11, 2025] - Breakdown by view type
- HTML page views : 17446
- PDF downloads : 5135
