Make the best use of Scientific Research and information from our 700+ peer reviewed, Open Access Journals that operates with the help of 50,000+ Editorial Board Members and esteemed reviewers and 1000+ Scientific associations in Medical, Clinical, Pharmaceutical, Engineering, Technology and Management Fields.
Meet Inspiring Speakers and Experts at our 3000+ Global Conferenceseries Events with over 600+ Conferences, 1200+ Symposiums and 1200+ Workshops on Medical, Pharma, Engineering, Science, Technology and Business
Review Article Open Access
Long Term Outcomes of Laparoscopic Adjustable Gastric Banding for Treatment of Morbid Obesity in Adolescents
| Chrestiana Dewi1* and Sucandy Iswanto2 | |
| 1Abington Memorial Hospital, Department of Surgery, Abington, PA, USA | |
| 2Airlangga University School of Medicine, Surabaya, Indonesia | |
| Corresponding Author : | Dewi Chrestiana, M.D Department of Surgery Abington Memorial Hospital Abington, 117 N Easton Road Glenside PA 19038, USA Tel: 215-429-6400 E-mail: dewichrestiana@yahoo.com |
| Received April 29, 2013; Accepted May 10, 2013; Published May 13, 2013 | |
| Citation: Dewi C, Iswanto S (2013) Long Term Outcomes of Laparoscopic Adjustable Gastric Banding for Treatment of Morbid Obesity in Adolescents. J Obes Weight Loss Ther 3:175. doi:10.4172/2165-7904.1000175 | |
| Copyright: © 2013 Dewi C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Obesity & Weight Loss Therapy
| Childhood obesity becomes a concern to parents and health providers. Children with body mass index (BMI) >99th percentile tends to become obese adults with more health complications and higher mortality rate than those who become obese in adulthood. Nonoperative management through a well supervised diet, psychological counseling, and physical activity program have been shown to result in poor long-term sustainability and low success rate in significant percentage of adolescents [1,2]. A minimally invasive procedure without alteration in the anatomy of the gastrointestinal tract is considered more appropriate and less risky. Laparoscopic adjustable gastric banding (LAGB), therefore, has rapidly become the preferred bariatric operation for adolescents. Despite promising short-term results, little is known about its long term outcomes. We designed a study to review long term outcomes of LAGB in morbidly obese adolescents to understand the procedure benefits and to delineate its role in the treatment of childhood obesity. |
| Using PubMed, MEDLINE, and CHINAHL databases, metaanalytic review of 13 articles from 2005 to 2012 was performed (Table 1). Keywords used were adolescent, children, and laparoscopic gastric banding. The primary endpoint was long-term weight loss outcomes of LAGB for treatment of morbid obesity in adolescents. |
| Five hundred ninety one morbidly obese adolescents were included with equal gender distribution. The average preoperative BMI was 46.5 kg/m2. Preoperative obesity-related co morbidities included steatohepatitis (80.8 ± 14.3%), dyslipidemia (55.1 ± 29.4%), diabetes mellitus (DM) (51.0 ± 44.1%), hypertension (HTN) (38.9 ± 24.7%), polycystic ovary syndrome (PCOS) (34.4 ± 11.9%), obstructive sleep apnea (OSA) (30.7 ± 15.8%), depression (26.9 ± 4.2%), osteoarthritis (OA) (22.5 ± 19.5%), and gastroesophageal reflux disease (GERD) (12.2 ± 15.5%). The mean operative time was 62.7 minutes and the length of hospital stay was 32.9 hours. At 6, 12, 18, 24, 36, 48, and 60 months after the LAGB, the average excess weight loss were 29.1%, 44%, 57.8%, 51%, 60.8%, 63%, and 66.2%, respectively (Table 2). All of the comorbidities were improved or resolved postoperatively. Postoperative complications were reported in 76 patients (12.3%), which included band slippage ± pouch dilation 30 (39.47%), vitamin or mineral deficiency 11 (14.5%), subcutaneous port complications requiring revision 8 (10.5%), severe gastro esophageal reflux 5 (6.6%), dehydration 4 (5.3%), band leakage 3 (3.9%), and others. |
| Morbidly obese adolescents with multiple obesity-related co morbidities are at risk for suboptimal performance and development during their adulthood. Childhood obesity is associated with steatosis, dyslipidemia, type 2 diabetes, hypertension, polycystic ovary, obstructive sleep apnea, depression, nonalcoholic fatty liver, orthopedic problems, gastroesophageal reflux disease, coronary artery disease, fatty liver disease, and premature mortality in adulthood. Obesity causes vessels rigidity especially carotid artery, which subsequently causes hypertension and cardiovascular disease. Consequence of obstructive sleep apnea presents as learning difficulties, hyperactivity, and cardiovascular abnormalities. Depression brings a concern where it is accompanied by potentially dangerous behaviors such as feelings of guilt, anxiety, panic, paranoia, alcohol use, tobacco use, illicit drug use, suicidal ideation, suicidal attempts, and deliberate self-harm [3]. |
| Surgical weight loss method has been known to be the most effective and durable treatment for morbid obesity. O’Brien et al. reported in their study of randomized controlled trial comparing gastric banding procedure versus a lifestyle weight loss program [1]. The extent of weight loss, resolution of metabolic syndrome and insulin resistance were substantially greater in the gastric banding group. The variability in the rate of weight loss between time periods was observed and it is thought to be related to uncontrolled diet, lack of exercise or psychological support [1,4-6], and loss of follow-up [7,8]. A combination of surgical procedure, exercise program and lifestyle modification produce the most optimal outcomes. Lack of social supports, failure to change eating habits, and failure to incorporate recommended exercise are the most common causes of suboptimal weight loss following LAGB. Overall complication after LAGB was 12.3% (Figure 1). Band slippage with or without pouch dilation was the most common complication after LAGB. Yitzhak et al. and Fielding et al. proposed the solution for this problem by utilizing pars-flaccida approach to the esophagogastric angle. This method reduced the incidence of band slippage from 28% to <3% [2] and from 12% to 1-2% [9], respectively. Of the total patients, only eleven (1.8%) experienced vitamin or mineral deficiency. Appropriate supplementation before symptoms development effectively prevents this complication. Gastroesophageal reflux and inability to tolerate oral diet resulting in dehydration can be managed by adjusting the gastric banding during follow-up visits. Lack of experience in managing early port-related complications is associated with increased need for reoperation. Other reported minor complications include tube crack, port site bleeding or hematoma, superficial soft tissue infection, cholelithiasis and nephrolithiasis. |
| Morbidly obese adolescent who failed multiple attempts of nonoperative weight loss programs, potentially benefit from laparoscopic adjustable gastric banding. This procedure is safe, effective, and durable in achieving weight loss outcome, with acceptable rates of postoperative complications. Postoperative exercise program, lifestyle modification, and psychological support continue to play a major role in the ultimate success of the operation. |
References
- O'Brien PE, Sawyer SM, Laurie C, Brown WA, Skinner S, et al. (2010) Laparoscopic adjustable gastric banding in severely obese adolescents: a randomized trial. JAMA 303: 519-526.
- Yitzhak A, Mizrahi S, Avinoach E (2006) Laparoscopic gastric banding in adolescents. Obes Surg 16: 1318-1322.
- Duffecy J, Bleil ME, Labott SM, Browne A, Galvani C (2008) Psychopathology in adolescents presenting for laparoscopic banding. J Adolesc Health 43: 623-625.
- Silberhumer GR, Miller K, Pump A, Kriwanek S, Widhalm K, et al. (2011) Long-term results after laparoscopic adjustable gastric banding in adolescent patients: follow-up of the Austrian experience. Surg Endosc 25: 2993-2999.
- Zitsman JL, Fennoy I, Witt MA, Schauben J, Devlin M, et al. (2011) Laparoscopic adjustable gastric banding in adolescents: short-term results. J Pediatr Surg 46: 157-162.
- Silberhumer GR, Miller K, Kriwanek S, Widhalm K, Pump A, et al. (2006) Laparoscopic adjustable gastric banding in adolescents: the Austrian experience. Obes Surg 16: 1062-1067.
- Osorio A, Moreira-Pinto J, Pereira J, Silva G, Bonet B, et al. (2011) 9 Years after the first laparoscopic adjusted gastric banding (LAGB) in adolescents: the Portuguese experience. Eur J Pediatr Surg 21: 331-334.
- Nadler EP, Youn HA, Ginsburg HB, Ren CJ, Fielding GA (2007) Short-term results in 53 US obese pediatric patients treated with laparoscopic adjustable gastric banding. J Pediatr Surg 42: 137-141.
- Fielding GA, Duncombe JE (2005) Laparoscopic adjustable gastric banding in severely obese adolescents. Surg Obes Relat Dis 1: 399-405.
Tables and Figures at a glance
| Table 1 | Table 2 |
Figures at a glance
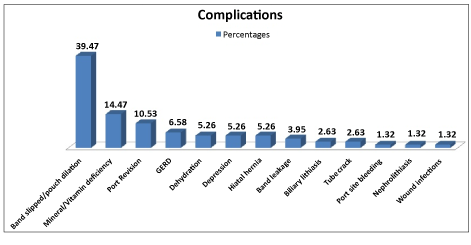 |
| Figure 1 |
Post your comment
Relevant Topics
- Android Obesity
- Anti Obesity Medication
- Bariatric Surgery
- Best Ways to Lose Weight
- Body Mass Index (BMI)
- Child Obesity Statistics
- Comorbidities of Obesity
- Diabetes and Obesity
- Diabetic Diet
- Diet
- Etiology of Obesity
- Exogenous Obesity
- Fat Burning Foods
- Gastric By-pass Surgery
- Genetics of Obesity
- Global Obesity Statistics
- Gynoid Obesity
- Junk Food and Childhood Obesity
- Obesity
- Obesity and Cancer
- Obesity and Nutrition
- Obesity and Sleep Apnea
- Obesity Complications
- Obesity in Pregnancy
- Obesity in United States
- Visceral Obesity
- Weight Loss
- Weight Loss Clinics
- Weight Loss Supplements
- Weight Management Programs
Recommended Journals
Article Tools
Article Usage
- Total views: 13058
- [From(publication date):
July-2013 - Apr 03, 2025] - Breakdown by view type
- HTML page views : 8552
- PDF downloads : 4506
