Case Report Open Access
Leclercia adecarboxylata: The First Reported Infection of Cerebrospinal Fluid and a Systematic Review of the Literature
| Jill P Stone1, Hannah St Denis-Katz2, Claire Temple-Oberle3*, Phillipe Mercier4, Jonah B Mizzau5 and Alim P Mitha4 | |
| 1Division of Plastic Surgery, Department of Surgery, University of Calgary, Calgary, Canada | |
| 2University of Saskatchewan, Canada | |
| 3Division of Surgical Oncology, Department of Surgery, University of Calgary, Calgary, Canada | |
| 4Department of Clinical Neurosciences, University of Calgary, Calgary, Canada | |
| 5Department of Internal Medicine, University of Calgary, Calgary, Canada | |
| Corresponding Author : | Claire Temple-Oberle Division of Surgical Oncology, Department of Surgery University of Calgary, 1331 29 St NW T2A4N2 Calgary, Canada Tel: 1403-220-5110 E-mail: Claire.Temple-Oberle@albertahealthservices.ca |
| Received: June 11, 2015 Accepted: July 19, 2015 Published: July 23, 2015 | |
| Citation: Stone JP, Denis-Katz HS, Temple-Oberle C, Mercier P, Mizzau JB, et al. (2015) Leclercia adecarboxylata: The First Reported Infection of Cerebrospinal Fluid and a Systematic Review of the Literature. J Neuroinfect Dis 6:181. doi:10.4172/2314-7326.1000181 | |
| Copyright: © 2015 Stone JP, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
| Related article at Pubmed, Scholar Google | |
Visit for more related articles at Journal of Neuroinfectious Diseases
Abstract
Background: Leclercia adecarboxylata is an emerging pathogen in the clinical setting. Initially considered an opportunist pathogen commonly associated with polymicrobial infections in immunocompromised individuals, recent evidence recognizes this pathogen in healthy individuals and with a growing antibiotic resistance profile. We report the first case of Leclercia adecarboxylata in cerebrospinal fluid of a young trauma patient and present a systematic review of the literature. Patient demographics and clinical history, outcomes and treatments are outlined. Methods: A systematic review identified relevant studies published through PubMed, Medline and ProQuest until July 2015. Search terms included “Leclercia adecarboxylata” and “Esherichia adecarboxylata”. Non-human cases and reports devoid of clinical infections were excluded. Results: A total of 40 articles (51 patients including the current case) were identified and included in our analysis. Patient age ranged from 24 weeks to 81 years old and included 18 female, 24 male, and 9 unknown. Immunocompromised (n=32) and healthy patients (n=15) revealed clinical isolates from blood and wound cultures most commonly (n=21 and 11). Sixteen isolates demonstrated antibiotic resistance. Thirty four cases were monomicrobial and fifteen were polymicrobial. Patient treatment and clinical outcome are reported. Conclusions: We present the most up to date review of Leclercia adecarboxylata infections. As the number of L. adecarboxylata cases continue to expand so does our insight into its pathogenicity and role in human clinical infections.
| Keywords |
| Leclercia adecarboxylata; Eschericia adecarboxylata; Cerebrospinal fluid; Infection |
| Background |
| Leclercia adecarboxylata was once thought to be a relatively uncommon pathogen [1]. Originally described by Leclerc in 1962 as Escherichia adecarboxylata, the development of more accurate identification methods reclassified this facultative aerobic, Gram negative bacillus as a member of the Enterobacteriaceae family [2]. It is a pathogen found widely in nature, having been isolated from food, water, and other environmental sources, as well as a commensal organism in the gut flora of some animals and humans [3-8]. This pathogen is often reported in immunosuppressed hosts and as part of polymicrobial infections [3]. It has been isolated from a number of specimens including blood; wound exudate, synovial, cerebrospinal, and peritoneal fluid [4]. We intend to present the most up to date summary of Leclercia adecarboxylata infections including patient demographics, details of clinical infection and treatment protocols. |
| Case Report |
| A previously healthy 32-year-old female pedestrian was struck by a motor vehicle at 35 miles/hr. Her injuries included skull fractures with intracranial bleeding and orthopaedic injuries. The patient required immediate EVD placement followed by hemicraniectomy and hematoma evacuation. On day three, routine culturing of EVD fluid yielded heavy Leclercia adecarboxylata found to be sensitive to ampicillin, ceftriaxone, gentamycin and meropenem. The infectious disease team recommended treatment with Meropenem (1 gram q8h). Multi-organ failure secondary to sepsis, declining neurological status and poor prognosis ultimately lead to the decision to withdraw care. On day 10 the patient was extubated and passed away. |
| Methods |
| Search strategy and selection criteria |
| A systematic review identified relevant studies published through PubMed, Medline and ProQuest until July 2015. Search terms included “Leclercia adecarboxylata” and “Esherichia adecarboxylata”. |
| All study types were included in the initial search, including abstracts and pending publications available. Non-electronic versions were requested. Bibliographies were reviewed to identify additional studies. Inclusion criteria required the publications to be pertaining to human subjects. Literature void of clinical infections were excluded. Non-English studies were excluded unless abstracts or translated data were available. |
| Two authors (J.S. and H.S.) independently reviewed the articles. Disagreements on consensus of inclusion or exclusion were arbitrated by a third author (J.M.). |
| Data extraction and outcomes |
| Title, author, journal and impact factor, publication year and study type were recorded. Data collected included the following: (1) Patient demographics (2) Past medical history (3) Clinical history surrounding infection (4) Co-infection of microorganisms (5) Antibiotic resistance (6) Intervention and treatment (7) Patient outcome. |
| Results |
| Study selection |
| Using the previously described search method, 165 articles were identified. Ninety-nine articles did not meet inclusion criteria and 40 duplicates were removed. The remaining 27 articles were screened by title and abstract. Review of the full articles yielded an additional twenty- three papers and secondary assessment of inclusion criteria excluded an additional five (Figure 1). |
| A total of 50 patients from 40 sources were included in our review. Six articles included more than one case [7,9-13]. The remaining 34 articles presented singular cases. Two case reports were published with reviews of the literature [4,6]. Eight patient cases were identified in the reviews of the literature that where unavailable to access (electronically, by loan, or no longer available in print) [12,14-18]. Data was extracted from these articles to be included in our analysis. No higher level of evidence publication was identified (case series and case reports only). |
| Study characteristics and quality assessment |
| Methodological quality assessment using Jadad composite scale and MINORS could not be completed due to the low level of evidence. A modified CARE (Case Report) checklist [19] for case report and journal impact factor were alternatively assessed to comment on quality. Impact factor of journals ranged from 0 - 9.177 (mean 2.39). The CARE checklist score ranged from 17-28 of the possible 30 points attainable. Patient cases identified in the reviews of the literature were included in our data extraction without being applied to the CARE checklist if they were unavailable. The Newcastle-Ottawa Assessment Scale (NOS) for assessing the quality of nonrandomized studies was applied to the case series retrieved [19]. The three themes, selection, comparability and exposure, were applied to Prakash, Anuradha, Temegsen, and Forrester, scoring two, three, four and two stars respectively. Other sources of potential bias were examined for during the course of our review and further outlined in the discussion. |
| Outcomes |
| Patient demographics and pertinent clinical data were extracted by two independent investigators and recorded in Table 1 [20-43]. Our case was included in the analysis that follows. Fifty-one cases comprised of eighteen female, twenty-four male, and nine unknown patients ranging in age from 24w to 81 years. Six pediatric patients were identified (24w, 26w, 8mo, 5yr, 8yr, 11yr). Four patient cases had no past medical history included and nine were reported as previously healthy. The remainder of the subjects (n=38, 71%) had concomitant comorbidities and/ or immunocompromised states. These included patients with history of substance abuse, patients undergoing chemotherapy, and chronic systemic diseases such as end-stage-renal-disease and cardiovascular disease (Table 1). Of the previously healthy patients, Leclercia isolates were identified in six wound cultures following trauma, in a tracheal aspirate, gluteal abscess aspirate, blood following a burn, stump wound, foot wound, and in the CSF fluid of the current case presented. |
| Leclercia adecarboxylata was isolated from a variety of sources of which blood and wound cultures were most frequently (seventeen and eleven respectively). Thirty-four cases were monomicrobial and fifteen were polymicrobial (two not reported). |
| Twenty-six Leclercia isolates were susceptible to all antimicrobials tested. Eight cases did not comment on antibiotic resistance and the remainder had varying resistance to sulfamethoxazole and trimethoprim, broad and extended spectrum beta-lactams, aminoglycoside, cephalosporin, and fosfomycin antibiotics (Table 2). The majority of patients improved with the appropriate antibiotic course tailored to the microbe’s sensitivity profile. Antibiotic choice and duration of treatment are presented in Table 2 (duration or antibiotic choice not recorded if unavailable). There were four cases which resulted in death including the current case presented. |
| Discussion |
| Emerging antimicrobial resistance is beginning to distinguish this as a potentially difficult pathogen [21]. Of the antimicrobial resistance profiles reported, nineteen were pansensitive. In vitro studies show this pathogen to be naturally resistant to lincosamides, ketolides, streptogramins, linezolid, glycopeptides, penicillin G, oxacillin, erythromycin, roxithromycin, clarithromycin, rifampicin, fusidic acid, and fosfomycin [22] The appearance of extended beta-lactamase resistance proves to pose a threat to clinicians in their treatment choices [23]. An optimal antibiotic regime has not been established for this pathogen as of yet, but with further research and clinical experience one can be founded [24]. The clinician should be aware of the emergence of resistance Leclercia strains and tailor treatments based on sensitivities of their case at hand. |
| Leclercia adecarboxylata is often described as an opportunistic pathogen [3]. The majority of patients had underlying medical issues or immunocompromised states. These included alcohol abuse, cancer, and chronic systemic diseases such as end-stage-renal-disease and cardiovascular disease. Our study highlights this rare pathogen as a cause of infection predominantly in the immunocompromised host as other authors have previously suggested. Of absolute paramount, Leclercia adecarboxylata also is a threat in previously healthy patients |
| Leclercia adecarboxylata was initially believed to be dependent on co-infecting microorganisms [23]. Our review reveals that the majority were monomicrobial infections (26 of 42 reported, 64%). This may be underreported as not all papers commented on the absence of other microorganism (n=2). It seems unlikely that this microorganism is dependent on co-infection and as such, we do not agree that its infectious role is contingent on other microorganisms [2]. We cannot support previous claims that infections were synergistically working together to enhance overall virulence although logically, multiple infections may be more difficult to overcome [4]. |
| We report of the first cerebral spinal fluid infection with Leclercia adecarboxylata. Our case additionally highlights a monomicrobial infection in a formerly healthy patient, a demographic previously underappreciated in the literature. |
| Conclusion |
| As the number of L. adecarboxylata infections continues to expand so does our insight into its pathogenicity and role in human clinical infections |
References
- Lee B, Sir JJ, Park SW, Kwak CH, Kim SM, et al. (2009) A case of Leclerciaadecarboxylata endocarditis in a woman with endometrial cancer. Am J Med Sci 337: 146-147.
- Shah A, Nguyen J, Sullivan LM, Chikwava KR, Yan AC, et al. (2011) Leclerciaadecarboxylata cellulitis in a child with acute lymphoblastic leukemia. PediatrDermatol 28: 162-164.
- Bali R, Sharma P, Gupta K, Nagrath S (2013) Pharyngeal and peritonsillar abscess due to Leclerciaadecarboxylata in an immunocompetant patient. J Infect DevCtries 7: 46-50.
- Forrester JD, Adams J, Sawyer RG (2012) Leclerciaadecarboxylata bacteremia in a trauma patient: case report and review of the literature. Surg Infect (Larchmt) 13: 63-66.
- Hess B, Burchett A, Huntington MK (2008) Leclerciaadecarboxylata in an immunocompetent patient. J Med Microbiol 57: 896-898.
- Michael Z, McGann PT, Alao O, Stevenson L, Lesho E, et al. (2013) Isolation of Leclerciaadecarboxylata from an infected war wound in an immune competent patient. Mil Med 178: e390-393.
- Anuradha M (2014) Leclerciaadecarboxylata isolation: case reports and review. J ClinDiagn Res 8: DD03-04.
- Kashani A, Chitsazan M, Che K, Garrison RC (2014) Leclerciaadecarboxylata Bacteremia in a Patient with Ulcerative Colitis. Case Rep Gastrointest Med 2014: 457687.
- Fernandez-Ruiz M, Lopez-Medrano F, Garcia-Sanchez L, Garcia-Reyne A, Ortuno de Solo T, et al. (2009) Successful management of tunneled hemodialysis catheter-related bacteremia by Leclerciaadecarboxylata without catheter removal: report of two cases. International Journal of Infectious Diseases 13:517-518.
- de Baere T, Wauters G, Huylenbroeck A, Claeys G, Peleman R, et al. (2001) Isolations of Leclerciaadecarboxylata from a patient with a chronically inflamed gallbladder and from a patient with sepsis without focus. J ClinMicrobiol 39: 1674-1675.
- Temesgen Z, Toal DR, Cockerill FR 3rd (1997) Leclerciaadecarboxylata infections: case report and review. Clin Infect Dis 25: 79-81.
- Cai M, Dong X, Wei J, Yang F, Xu D, et al. (1992) [Isolation and identification of Leclerciaadecarboxylate in clinical isolates in China]. Wei Sheng Wu XueBao 32: 119-123.
- Prakash MR, Ravikumar R, Patra N, Indiradevi B (2015) Hospital-acquired pneumonia due to Leclerciaadecarboxylata in a neurosurgical centre. J Postgrad Med 61: 123-125.
- Hwang HY, Jeong SH, Rim H, et al. (1998)A case of Leclerciaadecarboxylata isolated from dialysate in a patient with continuous ambulatory peritoneal dialysis. Korean ClinMicrobiol 1:11311-11316.
- Martínez MM, Sánchez G, Gómez J, Mendaza P, Daza RM (1998) [Isolation of Leclerciaadecarboxylata in ulcer exudate]. EnfermInfeccMicrobiolClin 16: 345.
- Dudkiewicz B, Szewczyk E (1993) [Etiology of bacterial endocarditis in materials from Cardiology and Cardiac Surgery Clinics of the Lodz Academy]. Med DoswMikrobiol 45: 357-359.
- Daza RM, Iborra J, Alonso N, Vera I, Portero F, et al. (1993) [Isolation of Leclerciaadecarboxylata in a cirrhotic patient]. EnfermInfeccMicrobiolClin 11: 53-54.
- Otani E, Bruckner DA (1991)Leclerciaadecarboxylata isolated from blood culture.ClinMicrobiolNewslett13:157-158.
- Gagnier JJ, Kienle G, Altman DG, Moher D, Sox H, et al. (2013) The CARE guidelines: consensus-based clinical case reporting guideline development. Headache 53:1541-1547.
- Stock I, Burak S, Wiedemann B (2004) Natural antimicrobial susceptibility patterns and biochemical profiles of Leclerciaadecarboxylata strains. ClinMicrobiol Infect 10: 724-733.
- Keren Y, Keshet D, Eidelman M, Geffen Y, Raz-Pasteur A, et al. (2014) Is Leclerciaadecarboxylata a new and unfamiliar marine pathogen? J ClinMicrobiol 52: 1775-1776.
- Haji S, Kimura H, Yamashita H (2014) Arthritis and bacteremia due to Leclerciaadecarboxylata. Intern Med 53: 2659.
- Chao CT, Hung PH, Huang JW, Tsai HB (2014) Cycler cassette rupture with Leclerciaadecarboxylata peritoneal dialysis peritonitis. Perit Dial Int 34: 131-132.
- De Mauri A, Chiarinotti D, Andreoni S, Molinari GL, Conti N, et al. (2013) Leclerciaadecarboxylata and catheter-related bacteraemia: review of the literature and outcome with regard to catheters and patients. J Med Microbiol 62: 1620-1623.
- Nelson MU, Maksimova Y, Schulz V, Bizzarro MJ, Gallagher PG (2013) Late-onset Leclerciaadecarboxylata sepsis in a premature neonate. J Perinatol 33: 740-742.
- Tam V, Nayak S (2012) Isolation of Leclerciaadecarboxylata from a wound infection after exposure to hurricane-related floodwater. BMJ Case Rep 2012.
- Shin GW, You MJ, Lee HS, Lee CS (2012) Catheter-related bacteremia caused by multidrug-resistant Leclerciaadecarboxylata in a patient with breast cancer. J ClinMicrobiol 50: 3129-3132.
- Myers KA, Jeffery RM, Lodha A (2012) Late-onset Leclerciaadecarboxylata bacteraemia in a premature infant in the NICU. ActaPaediatr 101: e37-39.
- Dalamaga M, Pantelaki M, Karmaniolas K, Daskalopoulou K, Migdalis I (2009) Isolation of Leclerciaadecarboxylata from blood and burn wound after a hydrofluoric acid chemical injury. Burns 35: 443-445.
- Dalamaga M, Pantelaki M, Papadavid E, Daskalopoulou K, Karmaniolas K (2008) [Epididymo-orchitis and bacteremia caused by Leclerciaadecarboxylata]. Med Mal Infect 38: 674-675.
- Corti G, Mondanelli N, Losco M, Bartolini L, Fontanelli A, et al. (2009) Post-traumatic infection of the lower limb caused by rare Enterobacteriaceae and Mucorales in a young healthy male. Int J Infect Dis 13: e57-60.
- Kim, H, Chon C, Ahn S, Jung S, Han K, et al. (2008) Fatal spontaneous bacterial peritonitis by Leclerciaadecarboxylata in a patient with hepatocellular carcinoma. International journal of clinical practice 62:1296-1298.
- JoverSáenz A, Cerezo-Esforzado E, Barcenilla-Gaite F, Garrido-Calvo S, Porcel- Pérez J (2008)Leclerciaadecarboxylatacholecystitis in a patient with metabolic syndrome. Surgical infections 9:411-412.
- Sawamura H, Kawamura Y, Yasuda M, Ohkusu K, Takahashi Y, et al. (2005) [A clinical isolate of Leclerciaadecarboxylata from a patient of pyelonephritis]. KansenshogakuZasshi 79: 831-835.
- Beltrán A, Molinero AV, Capilla S, Polo AM (2004) [Isolation of Leclerciaadecarboxylata from wound exudate of a diabetic patient]. Med Clin (Barc) 122: 159.
- Mazzariol A, Zuliani J, Fontana R, Cornaglia G (2003) Isolation from blood culture of a Leclerciaadecarboxylata strain producing an SHV-12 extended-spectrum beta-lactamase. J ClinMicrobiol 41: 1738-1739.
- Pérez-Moreno MO, Anguera J, Carulla M, Pérez-Moreno M (2003) [Septic arthritis due to Leclerciaadecarboxylata of probable iatrogenic origin]. EnfermInfeccMicrobiolClin 21: 167-168.
- Rodríguez JA, Sánchez FJ, Gutiérrez N, García JE, García-Rodríguez JA (2001) [Bacterial peritonitis due to Leclerciaadecarboxylata in a patient undergoing peritoneal dialysis]. EnfermInfeccMicrobiolClin 19: 237-238.
- Longhurst CA, West DC (2001) Isolation of Leclerciaadecarboxylata from an infant with acute lymphoblastic leukemia. Clin Infect Dis 32: 1659.
- Fattal O, Deville JG (2000) Leclerciaadecarboxylata peritonitis in a child receiving chronic peritoneal dialysis. PediatrNephrol 15: 186-187.
- De la Obra P, Domingo D, Casaseca R, Del Rey M, Lopez-Brea M (1999) Bacteremia due to Leclerciaadecarboxylata in a patient with multiple myeloma. ClinMicrobiol Newsletter 21:142-3.
- Lee NY, Ki CS, Kang WK(1999) Hickman catheter-associated bacteremia by Leclerciaadecarboxylata and Escherichia hermannii: A case report. Korean J Infect Dis 31:167-170.
- www.ohri.ca/programs/clinical_epidemiology/oxford.asp
Tables and Figures at a glance
| Table 1 | Table 2 |
Figures at a glance
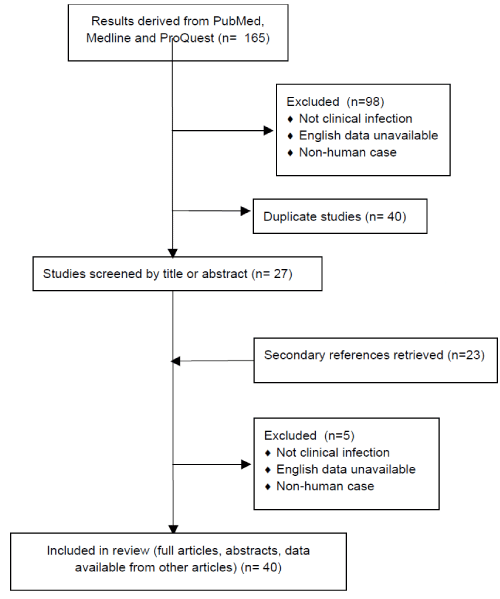 |
| Figure 1 |
Relevant Topics
- Bacteria Induced Neuropathies
- Blood-brain barrier
- Brain Infection
- Cerebral Spinal Fluid
- Encephalitis
- Fungal Infection
- Infectious Disease in Children
- Neuro-HIV and Bacterial Infection
- Neuro-Infections Induced Autoimmune Disorders
- Neurocystercercosis
- Neurocysticercosis
- Neuroepidemiology
- Neuroinfectious Agents
- Neuroinflammation
- Neurosyphilis
- Neurotropic viruses
- Neurovirology
- Rare Infectious Disease
- Toxoplasmosis
- Viral Infection
Recommended Journals
Article Tools
Article Usage
- Total views: 17537
- [From(publication date):
August-2015 - Jul 15, 2025] - Breakdown by view type
- HTML page views : 12878
- PDF downloads : 4659
