Inpatient Admissions after Aden Tonsillectomies for Pediatric Sleep-Disordered Breathing: Age as a Risk Factor
Received: 01-Jun-2022 / Manuscript No. ocr-22-65525 / Editor assigned: 03-Jun-2022 / PreQC No. ocr-22-65525 / Reviewed: 20-Jun-2022 / QC No. ocr-22-65525 / Revised: 25-Jun-2022 / Manuscript No. ocr-22-65525 / Accepted Date: 28-Jun-2022 / Published Date: 30-Jun-2022 DOI: 10.4172/2161-119X.1000469
Abstract
Objectives: The aim of this study was to analyze the incidence of post-operative respiratory complications in children aged 0-18 who underwent tonsillectomy and required inpatient hospital admission to determine the necessity of inpatient management for children under 3 years of age as outlined in the AAO-HNS clinical guidelines.
Methods: This was a single center, retrospective chart review. Inclusion criteria were pediatric patients who underwent tonsillectomies over a 4-year time span that were ages 0-18 and required inpatient admission after surgery. Post-operative parameters collected included respiratory rate, heart rate, and oxygen saturations. Also examined were the complications of bleeding and dehydration. Chi-squared tests were performed to look for statistical significance with p<0.05 considered statistically significant.
Results: The study sample included 64 patients; and the mean age was 5.2 years old. The most common comorbidities included OSA, asthma, obesity, and anatomical abnormalities. Only five distinct patients had vital sign abnormalities such as tachycardia, tachypnea, and oxygen saturations <90%. Most of these patients had complex comorbidities which affected their post-operative course, including Trisomy 21, Noonan syndrome, macrocephaly, and laryngomalacia. The chi-squared test to determine the relationship between age group (age ≤3, age 4-11, age 12-18) and presence of complications revealed a p value of 0.90. This suggests that there is no statistically significant difference between the age groups in risk of having respiratory complications. There were no children under the age of 3 who were otherwise healthy with no comorbidities who had post-operative complications.
Conclusion: Children <3 years of age had no significant increase in risk of respiratory complications after tonsillectomy surgery. Comorbidities such as craniofacial malformations were more indicative of respiratory complications rather than age. Thus, decisions to admit a patient post-operatively should be made on a case-bycase basis depending on comorbidities rather than admitting all patients under 3 years, allowing better utilization of hospital resources without compromising patient safety.
Keywords
Tonsillectomy, Obstructive Sleep Apnea, Sleeps Disordered Breathing, Inpatient, Complications
Introduction
Aden tonsillectomies are one of the most common surgeries performed in the United States in the pediatric population, with over 200,000 procedures each year in children <15 years of age [1]. The two major clinical indications for the procedure include the spectrum of obstructive sleep disordered breathing (SDB) and recurrent throat infections. Complications, though rare, include intraoperative and postoperative hemorrhage (primary within 24 hours of surgery, secondary up to two weeks after surgery), infection, dehydration and trauma to nearby structures [2]. This common procedure has significant effects on costs in the health care system, and there are significant differences in cost for same day outpatient surgery versus post-surgery hospital admission.
The surgery is generally very successful at improving many outcomes, such as better sleep, decreased infections (tonsillitis), improved school performance, less behavioral problems, less asthma exacerbations, and more. The Agency for Healthcare Research and Quality review demonstrated that tonsillectomy can lead to improvement in sleep outcomes as compared with no surgery in children with oSDB [3]. Other studies have found that behavioral parameters and school performance also improve after resolution of oSDB. Thus, this surgery can profoundly impact the growth and development of a child, and thus can be recommended to children, given proper indications and health status.
Before performing a tonsillectomy, children with oSDB are referred for polysomnography if they are <2 years of age or have certain comorbidities such as Down syndrome, craniofacial abnormalities, neuromuscular disorders, or sickle cell disease. Polysomnography confirms the severity of obstructive sleep apnea (OSA) and the appropriateness of doing a tonsillectomy. Mild OSA is defined by an obstructive AHI of 1 to <5 events/hour; moderate OSA is defined as an AHI>5 and <10 events/hour; and severe OSA is defined as AHI>10 events/hour.
In 2018, the American Academy of Otolaryngology-Head and Neck Surgery Foundation updated their guidelines regarding tonsillectomies in children [4]. Key Action Statement 12 was a newly added guideline and states the recommendation: “Clinicians should arrange for overnight, inpatient monitoring of children after tonsillectomy if they are <3 years old or have severe obstructive sleep apnea (apneahypopnea index >10 obstructive events/hour, oxygen saturation nadir <80% or both).” This particular guideline was compiled based on Grade B evidence quality: observational studies on age, meta-analysis of observation studies regarding complications. The benefits were to improve patient safety and satisfaction that would allow prompt detection and management of respiratory complications among highrisk children. The risks and costs included unnecessary admission of children who are low risk, occupying a hospital bed in limited resource settings, risk of iatrogenic injury, and cost of hospital care. The level of confidence in evidence was Medium, and it was determined that there was a preponderance of benefit over harm.
The objective of this study is to add to existing knowledge of the necessity to recommend inpatient monitoring post-surgery for children <3 and with moderate or severe sleep apnea. Our hypothesis was that children younger than 3 years of age who were otherwise healthy without any comorbidity or documented severe sleep apnea by sleep studies may not need postoperative admission after adenotonsillectomy. The results of this study can help guide decisions that pediatric otolaryngologists make, while justifying more outpatient tonsillectomies and reducing hospital costs.
Material And Methods
The objectives were studied by conducting a single-center retrospective chart review of pediatric patients who had a tonsillectomy or adenotonsillectomy at the University of Massachusetts Medical Center in Worcester, Massachusetts. Records collected were for patients who had surgery in the main hospital operating room between October 1, 2017- July 1, 2021. The inclusion criteria included children ages 0-18 with a tonsillectomy or adenotonsillectomy who were admitted to the hospital after surgery. To eliminate possible confounding of the surgeon’s personal techniques in the tonsillectomies, all patients chosen for the study were operated on by the same otolaryngologist. Children
Using the electronic medical record, chart review was conducted to collect patient demographics such as age, gender, and comorbidities. The indication for inpatient admission was also recorded, whether it was due to age
Results
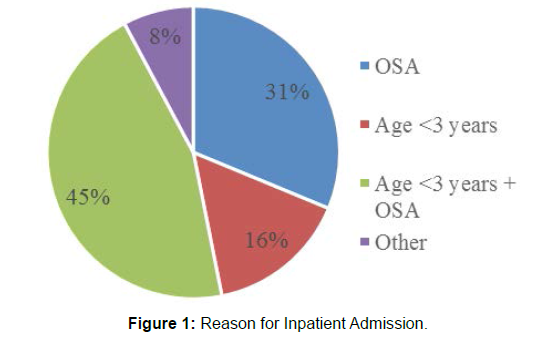
Between October 1, 2017 and July 1, 2021, there were 64 patients who met the inclusion criteria. The mean age of the patients was 5.2 years old, with a mode of 2 years and median of 2 years. They ranged from 19 months old to 17 years old. Seventy percent of patients were male, while 30% were female. The major indication for inpatient admission was patients that were less than 3 years of age and had OSA (45%). Thirty-one percent of patients were admitted because of a diagnosis of OSA, 16% due to their age <3, and 8% of patients due to other causes (Figure 1). This other causes included comorbidities such as sickle cell disease which required pre-operative blood transfusion. The most common comorbidities Table 1 included OSA, asthma, obesity, and anatomical abnormalities (including Trisomy 21, microcephaly, Noonan syndrome, laryngomalacia, micro deletion of chromosome 19p). The majority of patients stayed overnight for just one day, with only 8 patients (12.5%) staying inpatient for 2 days before discharge. These included children who had hematologic conditions such as sickle cell disease or Von Will brand’s Disease, along with those patients who had post-operative complications.
| Comorbidity | Prevalence (n) |
|---|---|
| Obstructive Sleep Apnea | 42 |
| Obesity | 10 |
| Anatomical Abnormality (trisomy 21, Noonan yndrome, etc.) | 6 |
| Hematological (sickle cell disease, VWD) | 4 |
| Asthma | 12 |
Table 1: Common Comorbidities Prevalence.
Looking at postoperative measures, in total, these were five unique patients who had post-operative vital sign abnormalities such as tachycardia, tachypnea, oxygen saturations <90%. Most of these patients had complex comorbidities which affected their postoperative course. One patient was a 2-year-old female patient with congenital hypothyroidism, Trisomy 21, and asthma, who required 2 racemic epinephrine nebulizers, blow-by oxygen, and observation in the PICU. Another was a 2-year-old male patient with macrocephaly, developmental delay, and a micro deletion of chromosome 19p, and he required blow-by oxygen and PICU observation. Another 2-year-oldmale with developmental delay, laryngomalacia, and a cardiac murmur also had post-operative tachypnea and oxygen saturations <95%, needing high-flow nasal cannula and BiPAP. A 9-year-old female with Noonan syndrome and OSA also had respiratory distress following her surgery, but required no intervention. A 13-year-old male with OSA and autism had some respiratory distress which resolved with dexamethasone administration for suspected pharyngeal/laryngeal edema. Therefore, only patients with comorbidities as above had postoperative respiratory complications. All other children had no vital sign abnormalities after surgery.
Running statistical tests showed the significance of the gathered data (Table 2). The chi-squared test to determine the relationship between age group (age ≤3, age 4-11, age 12-18) and presence of complications revealed a p value of 0.90. This suggests that there is no statistically significant difference between the age groups in risk of having complications, further supporting the idea that all children under 3 may not need to be admitted. Additionally, there was no significant difference in incidence of complications between male and female patients. (p=0.41).
| Age | Total (n) | Complications (n) | No complications (n) | p-value (0.90) |
|---|---|---|---|---|
| £ 3 years | 40 | 3 | 37 | |
| 4-11 years | 13 | 1 | 12 | |
| 12-18 years | 11 | 1 | 10 | |
| Gender | 0.41 | |||
| Male | 45 | 3 | 42 | |
| Female | 19 | 2 | 17 |
Table 2: Complication Rate by Groups.
Discussion
Based on the AAO-HNS guidelines, many institutions require overnight admission of young children <3 years of age and children with moderate to severe sleep apnea after a tonsillectomy. From the data at our single institution, we found that all children under 3 with no comorbidities did not have complications or require any interventions after their PACU stay, suggesting that they may not need to stay overnight.
A retrospective Study done by Colclasure et al. found that only 5 out of 3,340 outpatient T&A cases were identified as patients who would have been in the hospital at the time the complication occurred if all T&A patients had been hospitalized for 48 hours postoperatively [5, 6]. The authors determined that this is a risk level low enough to justify outpatient operations for most children, keeping in mind other factors such as comorbidities. A case-control study by Belyea et al. found that post-tonsillectomy complication rates in children under age 3 were low and no significant difference was observed between study and control groups. Just like the studies mentioned above, our study supports the idea that the guideline does not necessarily have to include children up to 3 years old, since many of them do not have complications. Imposing a lower age threshold for admission would be more cost-effective, without sacrificing patient care or putting children at higher risk.
In our study, there was no statistically significant increased risk of complications in kids <3, compared to older children. There have been some studies that demonstrate that age <3 is a risk factor for complications; a prospective cohort study mentioned in the AAO-HNS guidelines looked at predictors of perioperative complications in highrisk children after adenotonsillectomy [7]. The study demonstrated that 29% of children in higher risk population’s status post tonsillectomy had major respiratory complications. However, it is important to note that this higher risk group included children who were <3 years of age, obese, preterm, or had comorbidities. Also, the study was conducted at a tertiary center where the authors state there may have been a disproportionate number of high-risk children treated. Their results show that polysomnograms results may be a better predictor of perioperative complications and should be taken into account when choosing which children to admit or not admit overnight. Many of the children in our study did have polysomnograms, but others were diagnosed with OSA clinically and did not have a sleep study done prior to surgery.
Our study supports the idea that the AAO-HNS guideline may not be cost-effective, given the minimal chance of post-operative complications, even for children considered higher at risk. A study by Smith, et al. found that daily charge of admission at their institution averaged $1,823, and they found that following AAO-HNS guidelines, admissions would have cost $647,165 [8]. they concluded that more studies are needed to validate the current guidelines while also taking into account the burden on the health care system. Another study that surveyed centers around the country found that 44% of tertiary care children’s hospitals in the United States do not have an official admission policy to guide adenotonsillectomy care following the release of the 2011 AAO-HNS clinical practice guidelines, and even for institutions that do have an official admission policy, they are not universally aligned with the AAO-HNS guidelines [9]. The indications for admission varied, with 90% of respondents using criteria of age <3 years and neuromuscular disorders. Although this study was done before the addition of the 2019 guidelines, it demonstrates the uncertainty over indications for inpatient admissions, current practices, and the cost-benefit ratio.
Limitations of the study include small sample size, which may limit generalizability. Also, many patients did not have polysomnograms done prior to surgery, which would have provided more information regarding severity of their obstructive sleep apnea. Further studies with larger sample sizes may show significant differences in complications/ intervention rates between different study groups. Furthermore, this is a single-center retrospective chart review, and there may be differences in demographics due to geography and access to a tertiary care center. All patients included in the study were operated on by the same surgeon, so a larger study with patients treated by multiple providers would provide more generalizable results. Regardless, the results of this study can help aid in decision-making regarding inpatient admission for patients less than 3 years of age.
Conclusion
This retrospective chart review supports the idea that tonsillectomies can be performed with minimal complications and interventions in healthy children, even ages <3 years old. As such, it may not be necessary to utilize incredible hospital costs annually for such a common pediatric surgery that has very low chance of complications in otherwise healthy children. However, it is important to consider each admission on a case-by-case basis, taking into account comorbidities of children that may affect their post-operative course. Preoperative patient selection is very important. We think that the majority of elective admission under 3 years of age without the diagnosis of severe sleep apnea or any other comorbidity met the criteria for same- day discharge. For patients <3 years who are otherwise healthy, otolaryngologists could perform reevaluation 4 to 6 hours after surgery for possible discharge home the same day, alongside shared decision-making with the parents. Patient safety is the utmost importance, but decreasing medical costs for both the patients and the hospitals would lead to a more efficient utilization of resources with redistribution of funds for other necessary functions.
Acknowledgement
None
Declarations of interest
None
References
- Mitchell RB, Archer SM, Ishman SL, Rosenfeld RM, Coles S et al. (2019) Clinical Practice Guideline: Tonsillectomy in Children (Update)-Executive Summary. J Amer Acad Otolaryngol Head Neck Sur 160: 187-205.
- Windfuhr JP, Chen YS, Remmert S (2006) Hemorrhage following tonsillectomy and adenoidectomy in 15,218 patients. Otolaryngol Head Neck Surg 132:281-286.
- Francis DO, Chinnadurai S, Sathe N, et al. (2017) Tonsillectomy for Obstructive Sleep-Disordered Breathing or Recurrent Throat Infection in Children. Agency for Healthcare Research and Quality comparative effectiveness review 16- EHC042-EF.
- Schwengel DA, Sterni LM, Tunkel DE, Heitmiller ES (2009) Perioperative management of children with obstructive sleep apnea. Anesth Analg 109:60-75.
- Colclasure JB, Graham SS (1990) Complications of outpatient tonsillectomy and adenoidectomy: a review of 3,340 cases. Ear Nose Throat J 69:155-160.
- Belyea J, Chang Y, Rigby MH, Corsten G, Hong P (2014) Post-tonsillectomy complications in children less than three years of age: a case-control study. Int J Pediatr Otorhinolaryngol 78:871-874.
- Thongyam A, Marcus CL, Lockman JL, Cornaglia MA, Caroff A, et al. (2014) Predictors of perioperative complications in higher risk children after adenotonsillectomy for obstructive sleep apnea: a prospective study. Otolaryngol Head Neck Surg 151:1046-1054.
- Smith DF, Spiceland CP, Ishman SL, Engorn BM, Donohue C, et al. (2017) Admission criteria for children with obstructive sleep apnea after adenotonsillectomy: considerations for cost. J Clin Sleep Med 13:1463-1472.
- Nardone HC, McKee-Cole KM, Friedman NR (2016) Current Pediatric Tertiary Care Admission Practices Following Adenotonsillectomy. JAMA Otolaryngol Head Neck Surg 142:452-456.
Indexed at, Google Scholar, Crossref
Indexed at, Google Scholar, Crossref
Indexed at, Google Scholar, Crossref
Indexed at, Google Scholar, Crossref
Indexed at, Google Scholar, Crossref
Indexed at, Google Scholar, Crossref
Citation: Doshi M, Kamil S (2022) Inpatient Admissions after Aden Tonsillectomies for Pediatric Sleep-Disordered Breathing: Age as a Risk Factor. Otolaryngol (Sunnyvale) 12: 469. DOI: 10.4172/2161-119X.1000469
Copyright: © 2022 Doshi M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 1622
- [From(publication date): 0-2022 - Apr 05, 2025]
- Breakdown by view type
- HTML page views: 1289
- PDF downloads: 333