Research Article Open Access
Evaluation of Trans-Aortic Oblique Fluoroscopic Tunnel Vision Approach of Celiac Plexus Block after Failure of the Classic Approach
| Dina Nabil Abbas* | |
| Department of Anesthesiology, ICU and Algology Department, National Cancer Institute, Cairo University, Egypt | |
| Corresponding Author : | Dina Nabil Abbas Department of Anesthesiology ICU and Algology Department, National Cancer Institute Cairo University, Egypt, E-mail: dinanabil1@yahoo.com |
| Received December 10, 2012; Accepted January 20, 2012; Published January 27, 2012 | |
| Citation: Abbas DN (2012) Evaluation of Trans-Aortic Oblique Fluoroscopic Tunnel Vision Approach of Celiac Plexus Block after Failure of the Classic Approach. J Pain Relief 1:103. doi: 10.4172/2167-0846.1000103 | |
| Copyright: © 2012 Abbas DN. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Pain & Relief
Abstract
The conventional techniques of neurolytic celiac plexus block (NCBP) sometimes cannot be used in patients who have organomegaly, or not be able to tolerate the prone position necessary to place the needles; also anatomic anomalies may hinder obliquely placed needles from effectively reaching the target area. Complications such as organ puncture cannot be avoided with conventional techniques. The purpose of this study was to evaluate the safety and efficacy of a single needle transaortic celiac plexus block under an oblique tunnel view fluoroscopic guidance approach of celiac plexus alcohol block.
Fifty patients with advanced upper abdominal cancer in whom the classic celiac plexus block failed were included in the study. A percutaneous single needle transaortic celiac plexus block under an oblique tunnel view fluoroscopic guidance was done at the level of middle L1 vertebra). Visual analog score, daily morphine consumption, duration of the procedure, adverse effects, and Quality of Life Questionnaire-QLQ-C30 were recorded. The mean visual analog score, daily morphine consumption significantly decreased and Quality of Life Questionnaire-C30 score significantly improved after the procedure.
Conclusion: The percutaneous single needle transaortic celiac plexus block under an oblique tunnel view fluoroscopic guidance approach for celiac plexus block for upper abdominal cancer pain is proved to be safe and reliable and can be used as an alternative to the classic approach.
| Keywords |
| Celiac plexus block; Oblique tunnel vision view; Abdominal cancer pain. |
| Introduction |
| Celiac plexus is the largest sympathetic nervous system plexus that innervates the upper abdominal organs (pancreas, diaphragm, liver, spleen, stomach, small bowel, ascending colon and proximal part of transverse colon, adrenal glands, kidneys, abdominal aorta. The celiac plexus is embedded in loose areolar tissue, lies within the retroperitoneal space posterior to the stomach and pancreas close to the celiac axis and is separated from vertebral column by crus of diaphragm. It overlaps the aorta at the level of first lumbar vertebra between the origin of celiac and superior mesenteric arteries. It is a dense ganglia around the aorta with considerable variability in size (0.5-4.5 cm), number 1-5 and position (T12 -L1 disc space to middle of L2 vertebral body). It receives Preganglionic sympathetic fibers from splanchnic nerves, Preganglionic parasympathetic from vagus, Sensory fibers from phrenic and vagus, afferent fibers concerned with nociception [1]. Neurolytic celiac plexus block (NCPB) is one of the effective modalities for relief of intractable intra-abdominal pain due to malignancy or chronic pancreatitis. Many accounts of NCPB using a variety of indication and techniques [2-5] were recorded since it was first described by Kappis in 1918 [6]. However, conventional techniques sometimes cannot be used in patients who have organomegaly or anatomic anomalies such as extensive retroperitoneal adenopathy or tumor burden may hinder obliquely placed needles from effectively reaching the target area [7]. Furthermore, complications such as pneumothorax, and liver or kidney puncture cannot be avoided with conventional techniques [7-9], paraplegia is a rare complication [8]. Above that many patients with advanced disease may not be able to tolerate the prone position necessary to place the needles, despite that the transdiscal approach [10], may avoid such complications but the risk of discitis, degeneration of the disc, or disc herniation cannot be ignored. The purpose of this study was to evaluate the safety and efficacy of a percutaneous single needle transaortic oblique fluoroscopic tunnel vision view of the needle at the middle of L1 vertebrae approach of celiac plexus alcohol block. |
| Patients and Methods |
| After approval of local ethics committee and obtaining informed consent, 50 patients with refractory intra-abdominal cancer pain were recruited from the National Cancer Institute clinic. Patients whom the classic approach had technical problems (patient can not lay prone, or due to organomegaly) or ineffective previous classic technique were included in the study. Patients who had any contraindications to regional blockade (coagulopathy, local infection at area of needle insertion, and mental disorders) were excluded from the study. VAS score and Quality of Life Questionnaire (QLQ-C30) 11 were assessed before the procedure. The QLQ-C30 (version 3.0) is an integrated system by European Organization for Research and Treatment of Cancer for assessing the quality of life and is designed for use with a wide range of cancer patient Populations; it is composed of both multi item scales and single-item measures. It is grouped into five functional subscales (role, physical, cognitive, emotional and social functioning). In addition, there are three multi-item symptom scales (fatigue, pain, and nausea and vomiting), and two questions assessing overall QOL Each of the multi item scales includes a different set of items-no item occurs in more than 1 scale. All of the scales and single-item measures range in score from 0-100. A high scale score represents a higher response level. Thus, a high score for a functional scale represents a high/healthy level of functioning. A high score for the global health status/QoL represents a high QoL. A high score for a symptom scale/ item represents a high level of symptomatology/problems, a change in any scale of at least 10 points is considered to be clinically relevant 11. |
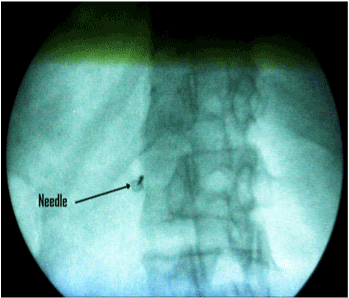
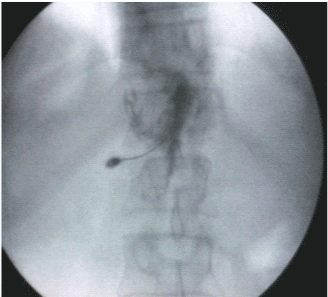
| Heart rate, noninvasive blood pressure, and oxygen saturation monitor were applied before and during the procedure. An intravenous catheter (18G) was inserted in a peripheral vein. One gram of ceftriaxone (Rocephin) was given intravenously 30 minutes before performing the procedure; also one liter of a crystalloid solution was infused during the procedure. Midazolam 0.03 mg/kg and fentanyl 1 ug/kg were given intravenously for sedation. Usually, the blocks were performed with the patients in the prone position but if they could not tolerate the prone position, they were placed in the lateral position, and the block was performed using fluoroscopic guidance. We manipulated the C arm to coincide with the patient position (prone or lateral) to obtain anteroposterior view, to visualize T12-L1 disc, the fluoroscopy tube was angled in cranio-caudal axis to flatten the inferior end plate of T12 then the tube is angled 35 degree to the left (for patients lying in prone position) or the intensifier is rotated upward to obtain oblique view (for patients laying in lateral position) to make the superior pars in the mid line.(i.e. the left anterolateral border of the L1 vertebral body is aligned with the tip of the transverse process after the L1 vertebral body), A tunnel view was used for needle insertion. Target point in the tunnel vision was just lateral to the middle of L1 vertebra (Figure 1), local anesthesia was applied with 1% lidocaine, 5 ml at the needle insertion site, which was 2.5-4.0 cm from midline then we advanced the needle (15cm, 20G Chiba needle) till aortic pulsation detected then increased resistance with subsequent loss of resistance and cessation of blood flow from the needle; this means penetration of the anterior wall of aorta , 0.5-1 ml of omnipaque dye was injected which should remain at midline on the posteroanterior view (Figure 2). Lateral view should confirm preaortic T12-L2 spread (Figure 3), and is often pulsating; 20 ml of 75% ethyl alcohol was injected through the needle after a negative aspiration test. |
| Patients were observed closely in the recovery unit for 1 hour after the injection and returned to the ward and were noticed for side effects and pain relief. Gradual opioid withdrawal was done according to needs of the patients. Duration of the procedure was recorded. The analgesic efficacy of the block was evaluated by assessing VAS and the total morphine consumption, before the block, 24 hours, 1, 2, 4, and 8 weeks after the block. Quality of life was assessed by using QLQ-C30. This questionnaire was recorded before block, 1, 2, 4, and 8 weeks after the procedure: For the total QOL of each patient, the difference between the pretreatment score and a follow-up score will be derived and then the patient will be categorized into clinically significant improvement, clinically significant deterioration, or no change. If the positive difference is greater than the SEM, then the patient is classified as having clinically significant QOL improvement. If the negative difference is less than the standard error measurement, then the patient is classified as having clinically significant QOL deterioration. If the difference fails to meet either criterion, then the patient is classified as no change. Adverse effects related to the procedure such as needle induced pain, hypotension, diarrhea, and any motor disturbances were recorded in all patients. The procedure is considered successful if there is satisfactory pain relief VAS≤ 3 or reduction in the dose of morphine. |
| Statistical analysis |
| Statistical analysis was carried out using stat view for windows software package version 4.57 (APACUS concepts, Berkely, CA). Data were represented as means±SD, percentage, and number. Statistical analysis was performed using Wilcoxon signed-rank test for the VAS and QLQ-C30 score changed from the baseline. Morphine consumption was tested using paired t-test. Statistical significance was accepted for P value less than 0.05. |
| Results |
| Between November 2009 and April 2011, patients were enrolled at the National Cancer Institute. Demographic, clinical data, morphine consumption of the patients, and the mean duration of the procedure are shown in (Table 1). The success rate (satisfactory pain relief VAS ≤3) was achieved in 98% after one day and after one week and reduced to 92% after one month and 90% after 2 months. The mean VAS decreased significantly (P<0.05) immediately after injection compared with the preprocedural period and was sustained at all study periods (Table 2). The number of patients on morphine decreased significantly from 50 patients before the block to only13 patients at 1 week after the block, and 15 and 18patients at 1 and 2 months after the block respectively. At day 1, there was significant decrease (P<0.05) in the dose of morphine consumption to 75.6±13 mg compared with the preblock level and 1 week after the block, there was more decrease to 55.6±15 mg, and thereafter, morphine dosage was stabilized until 8 weeks after the block throughout the study. QLQ-C30 was improved significantly (P<0.05) throughout the study after the block (Table 3). |
| Discussion |
| Abdominal cancer patients may experience severe pain that is resistant to oral or parenteral opioids. In addition, excessive sedation or other side effects may limit the acceptability and usefulness of oral or parenteral opioids therapy. Neurolysis of the sympathetic axis appears to be a safe, cost-effective approach to treating visceral pain associated with cancer. The benefits include improved analgesia, reduced opioid consumption, favorable economic implications, and superior clinical effects due to the deleterious properties of high-dose chronic opioid therapy. Current knowledge and techniques to perform these blocks allow these procedures to be performed safely and expeditiously. Pain practitioners should consider the role of these blocks as adjuvant therapy for the optimal treatment of cancer pain. The positive effect of NCPB was demonstrated by many studies [11], lilemoe et al. [12] in 1993 in double blind randomized study compared chemical splanchnicetomy with 50% alcohol on patients with unresectable cancer pancreas with placebo, pain relief was significantly superior in the NCPB received patients compared with placebo. In a prospective, randomized study, Ischia et al. [13] evaluated the efficacy of three different approaches of NCPB in pancreatic cancer. Of 61 patients with pancreatic cancer pain, 29 (48%) experienced complete pain relief after the neurolytic block [14]. The remaining 32 patients (52%) required further therapy for residual visceral pain due to technical failure in 15 patients and neuropathic/somatic pains in 17 patients 15. |
| Moore [15], popularized the classic posterolateral approach with fluoroscopic or palpatory guidance to position needles on each side of the aorta. By using CT guidance, more precise needle placement and better spread of solution could be obtained [7]. The rate of initial pain relief immediately after block with the conventional method was 94% [4]. Matamala et al. [16] described the percutaneous anterior approach to the celiac plexus using radiographic or ultrasound guidance. This approach may involve penetration of liver, bowel, pancreas, or tumor, and its safety and efficacy have not been established. |
| The present study revealed significant pain relief in Patients whom the classic approach had technical problems (patient cannot lay prone, or due to organomegaly) or ineffective previous classic technique, This was demonstrated by decrease in both VAS and morphine consumption. Many patients may continue on morphine as the pain may be mixed and has somatic element. Patients had clinically significant QOL improvement. Improvement in quality of life may be explained by improvement of the immune system because of better control of pain and depression, and increased ambulation secondary to reduction of pain leading to decreased complications and adherence to palliative care [15]. Decreased opioid consumption may improve the quality of life by decreasing sedative effect of opioids and enhance the immune system as it was shown that opioids had negative effect on immunity at the cellular level [16]. This is mainly because this approach made it possible to place the tip of the needle in the area close to the anterior wall of the aorta, despite the abnormal retroperitoneal anatomy that may be present in some cases. Positioning the needle tip adjacent to the anterolateral wall of the aorta in this technique may have facilitated maximum spread of alcohol [17]. The celiac plexus lies over the anterolateral wall of the aorta bilaterally. While with the conventional bilateral approach [7] the tip of the needle is placed at the points posterior to the aorta on the left and posterior to the inferior vena cava on the right. In the trans-aortic approach by Ischia et al. [18] the needle tip may pierce the aorta from side to side and sometimes it is difficult to encounter the aorta and may need many trials. The insertion point in our method is significantly closer to the midline compared to the conventional methods, which facilitates the ideal positioning of the needle tip just anterior to the aorta and is easy to locate the aorta at this entry point. We did not do diagnostic block before neurolysis as the clinical role of diagnostic block prior to NCPB is questionable and not warranted in patients with terminal malignancy, Yeun et al. [19], concluded that, a positive response to diagnostic block correlates positively with NCPB for abdominal visceral pain secondary to malignancy whereas it is a poor predictor when the response is negative. |
| Side effects after the celiac plexus block with alcohol were observed in our technique as well as in the conventional methods [4,9]. These include postural hypotension and diarrhea or frequent bowel movement due to sympathetic nerve blockade. Needle induced pain was minimal as it was only single puncture at definite site with no need to manipulate the needle, no organ injury as no organ or other anatomic structures impede needle placement, while in the conventional approach, the needles may pass through the kidney when the distance from the spinal process of the vertebra to the needle insertion point is increased [7, 19]. The danger of kidney or liver puncture in this approach is almost negligible, because the needle insertion point in our approach is closer to the midline. In addition, needle placement requires less time and only a single needle was used. Mete et al. [7], reported paraparesis after NCPB he proposed that the mechanism for this rare but devastating complication is the neurotoxicity of phenol on spinal cord which may result from spasmotic effect of phenol on spinal feeding arteries [8]. Although paraplegia after celiac plexus block is a very rare complication, anterior spinal artery syndrome should be considered as a possible serious complication of this procedure. It is also important to reassess the needle placement if unusual events occur, such as pain or increase resistance to injection. |
| In conclusion, the single left tunnel vision oblique fluoroscopic transaortic approach for celiac plexus block is easy and effective and was performed in 50 patients without encountering technical difficulties and without serious complications and can be done as an alternative to classic approach in cases where the classic approach is technically difficult or failed to relieve pain. |
References
- Niv D, Gofeld M (2008) Lumbar Sympathetic Blocks. In: Raj P, Lou L, Erdine S, Staats PS, eds. Interventional Pain Management-Image Guided Procedures, (2nd edn), PA: WB Saunders/Elsevier, Philadelphia.
- Boas RA (1978) Sympathetic blocks in clinical practice. Int Anaesthesiol Clin 14: 149-157.
- Singler RC (1982) An improved technique for alcohol neurolysis of the celiac plexus. Anesthesiology 56: 137-141.
- Moore DC (1979) Celiac (splanchnic) plexus block with alcohol for cancer pain of the upper intra-abdominal viscera, Advances in Pain Research and Therapy. (2nd volume), Edited by Bonica JJ, Ventafridda V. New York, Raven.
- Yeager MP (1995) Morphine inhibits spontaneous and cytokine enhanced natural killer cell cytotoxicity in volunteers. Anesthesiology 85: 500-508.
- Kappis M (1918) Die Ansthesierung des Nervus Splanchnicus Zentralbl 45: 709.
- Ahmet Mete, lutfiye pirbudak cocelli, Ruveyda Olmez, Betul kocamer, (2011) Acute developing transient paraparesis after celiac plexus block: MRI findings. Eur J Radiol Extra 78: 35-37.
- Brown DL, Bulley CK, Quiel EL (1987) Nuerolytic celiac plexus block for pancreatic cancer pain. Anesth Analg 66: 869-873.
- Plancarte-Sanches R, Mayer-Rivera F, del Rocio Guillen Nunez M, Guajardo-Rosas J, Acosta-Qiroz CO (2003) Transdiscal percutaneous approach of splanchnic nerves. Cir Cir 71: 192-203.
- Aaronson NK, Ahmedzai S, Bergman B, Bullinger M, Cull A, et al. (1993) The European Organisation for Research and Treatment of Cancer QLQ-C30: A quality-of-life instrument for use in international clinical trials in oncology. J Natl Cancer Inst 85: 365-376.
- Mercadante S (1993) Coeliac plexus block versus analgesics in pancreatic cancer. Pain 52: 187-192.
- Lillemoe KD, Cameron JL, Kaufman HS, Yeo CJ, Pitt HA, et al. (1993) Chemical splanchnicectomy in patients with unresectable pancreatic cancer. A prospective randomized trial. Ann Surg 217: 447-457.
- Ischia S, Ischia A, Polati E, Finco G (1992) Three posterior percutaneous celiac plexus block techniques: a prospective randomized study in 61 patients with pancreatic cancer pain. Anesthesiology 76: 534-540.
- Polati E, Finco G, Gottin L, Bassi C, Pedrozoli E, et al. (1998) Prospective randomized double blind trial of neurolytic celiac block in patients with pancreatic cancer. Br J Surg 85: 199-201.
- Moore DC (1981) Celiac plexus block: A roentgen graphic, anatomic study of technique and spread of solution in patients and corpses. Anesth Analg 60: 369-379.
- Matamala AM, Lopez FV, Sanchez JLA, Bach LD (1989) Percutaneous anterior approach to the celiac plexus using ultrasound. Br J Anaesth 62: 637-640.
- Staats PS, Hekmat H, Sauter P, Lillemoe K, (2001) The effects of alcohol celiac plexus block, pain and mood on longevity in patients with unrespectable pancreatic cancer: a double blind, randomized, placebo controlled study. Pain Med 2: 28-34.
- Ischia S, Luzzani A, Ischia A, Faggion S (1983) A new approach to the neurolytic block of the coeliac plexus: The transaortic technique. Pain 16: 333-341.
- Yuen TS, Ng KF, Tsui SL. (2002) Neurolytic celiac plexus block for visceral abdominal malignancy: Is prior diagnostic block warranted? Anaesth Intensive Care 30: 442-448.
Tables and Figures at a glance
| Table 1 | Table 2 | Table 3 | Table 4 |
Figures at a glance
 |
 |
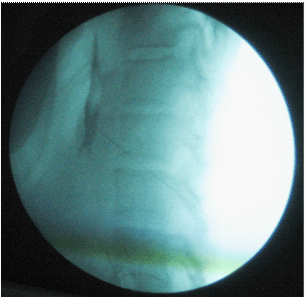 |
| Figure 1 | Figure 2 | Figure 3 |
Relevant Topics
- Acupuncture
- Acute Pain
- Analgesics
- Anesthesia
- Arthroscopy
- Chronic Back Pain
- Chronic Pain
- Hypnosis
- Low Back Pain
- Meditation
- Musculoskeletal pain
- Natural Pain Relievers
- Nociceptive Pain
- Opioid
- Orthopedics
- Pain and Mental Health
- Pain killer drugs
- Pain Mechanisms and Pathophysiology
- Pain Medication
- Pain Medicine
- Pain Relief and Traditional Medicine
- Pain Sensation
- Pain Tolerance
- Post-Operative Pain
- Reaction to Pain
Recommended Journals
Article Tools
Article Usage
- Total views: 15819
- [From(publication date):
February-2012 - Jul 06, 2025] - Breakdown by view type
- HTML page views : 11140
- PDF downloads : 4679
